Women of any age, but especially young women, mothers and women around the time of menopause, "perimenopause," need to take steps to prevent osteoporosis.
How to Prevent Osteoporosis
Given what we know today about osteoporosis, there is really no reason why contemporary young women should suffer the deformities and fractures of osteoporosis when they reach old age. Spine, hip and wrist fractures are not the inevitable consequences of aging. Proper diet, exercise and a number of new medications can be used for both prevention and treatment of primary osteoporosis. "Primary" osteoporosis refers to those cases where there are no other detectable causes, i.e., medications (steroids, anticonvulsants), endocrine conditions (hyperthyroidism or hyperparathyroidism) or bone disease, causing the bone loss.
In every woman, active bone formation occurs up to the age of 30, when she achieves peak bone mass. Thereafter, a gradual loss of bone begins until menopause, with an acceleration of bone loss for a period of about five years. Following that, there is again a gradual steady decrease. A woman who achieves a high peak bone density is much less likely to fall below the bone density level at which fracture risk becomes high.A woman who achieves a high peak bone density is much less likely to fall below the bone density level at which fracture risk becomes high.
Young women must adopt eating and exercise habits that contribute to bone formation. One half to one hour of weight bearing exercise three to six days per week, combined with adequate calcium intake, 1000-1500 mg/day, and vitamin D, 400-800 IU/day, are the most important building blocks of bone.
Diet Sodas and Couch Potatoes
Two trends in modern life are great hazards to bone formation: phosphoric acid-containing diet soda drinks and the sedentary lifestyle. Diet sodas have a high acid content that the body must neutralize with alkaline substances, notably calcium carbonate, which is leached from the bones. Frequently, girls and young women have made matters worse by trading in their milk for diet sodas and have thus deprived themselves of the single most important source of calcium. All women need milk products in their diets but it is especially critical for women who drink diet sodas. An 8 oz. glass of milk, 8 oz. of yogurt, a 1.5 oz. serving of cheese all provide 300 or more milligrams of calcium, providing a big boost to the daily requirement.
Whether the sedentary lifestyle happens in front of a TV screen or a computer terminal, it is still sedentary. But it is also true that too much exercise can backfire and interrupt bone mass build-up. Exercises that are associated with extreme thinness — distance running, gymnastics and ballet dancing — can lead to abnormally low estrogen levels with cessation of menstrual periods. This pseudo "post-menopausal state" can, by itself, produce further bone loss. The eating disorder, anorexia nervosa, contributes to bone loss by the same mechanism.
Tests to Detect Osteoporosis
Regular X-rays and DEXA (DXA)
If you have an X-ray that reveals osteoporosis, you've already had a 30-50% decrease in bone mass from the normal level. Plain X-rays are certainly not appropriate for screening for osteoporosis, since they reveal late-stage disease. The current best test is the "DEXA," Dual Energy X-ray Absorptiometry. This technique is becoming widely available. The standard test provides a density measurement of the lower spine and the thigh bone (femur).
These measurements are compared with a standardized measurement of a healthy 35-year-old woman, the T-score, and with the average for your age group, the Z-score. Your score may be expressed as a percentage of those numbers. Your scores can also be plotted on a graph (below) of bone mass densities (BMD) at various ages. The reports are impossible to read (even for doctors) but with a little detective work you can sort them out. On your own report, there will be a little star on the graph, indicating your density. You will be given one report for the hip and one for the spine.
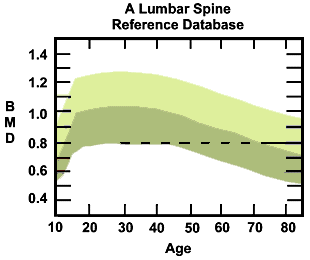
The dotted line in the graph is the fracture threshold. Note how more and more women fall below that line as they age. The light green area is two standard deviations (a measure of variation) above average and the dark green area, which is the one that concerns us, is two standard deviations below the average. As you can see, as women age, even average and above average BMDs can fall below the fracture line.
In your DEXA report, your BMD will be noted on this diagram by a star-like symbol. Your density will be compared with the average women in two ways. The Z-score compares you with the average women in your age group. The T-score compares you with the average young adult woman. Pay attention to the T-score.
You say to me, "That's not fair. I'm 55 and you want to compare me to a 35-year-old!" Actually that is just the point. This graph represents what is happening to women now. We don't want that. We want every women to achieve a high peak bone mass in her 20s and 30s and maintain it for the rest of her life. Then we would not have all these fractures and spinal deformities and disabilities and deaths attributable to osteoporosis.
The World Health Organization has developed definitions for degrees of bone loss. Normal is -1 standard deviation (SD) and above. Osteopenia (low bone mass) is -1.0 to -2.5 SD's. Osteoporosis is -2.5 SD's and below. An individual with -2.5 SD or below plus a history of weak bone related fracture is considered to have severe osteoporosis. You can tell where you are just by looking at the graph on your report.
DEXAs cost in the $100-300 range and may or may not be covered by insurance. Medicare is now covering bone density tests, so it is likely that the other insurers will follow. There are other tests for bone density, a type of CT (CAT) scan and ultrasound. If you have a screening test on the wrist or on the heel and it comes back low, my advice is to get a DEXA because, of all the tests, the DEXA is most accurate.
If you need follow up tests, have them done by the same technique (DEXA or CT) and the same type of machine (DEXA by Hologic or Lunar). Different tests and different types of machines do not give comparable results. The same principle is true for the next type of test.Medicare is now covering bone density tests, so it is likely that the other insurers will follow.
Bone Resorption Tests
Bone resorption tests, either in urine or blood, can also be useful. They measure how much breakdown of bone is occurring. The level can vary, depending on the time of day the test is taken. These tests are useful in monitoring therapy. A test may show high levels of breakdown that decrease after a particular medication is taken. Because of the variation in these tests, it is very important to have the same type of test done by the same laboratory, with the sample taken at the same time of day, in order for serial tests to be comparable.
When to Get Follow up Tests
Follow up tests are usually done to find out if lifestyle/diet changes or medications are stabilizing or improving bone density. DEXA's and CT's really cannot be done any more frequently than once a year because significant changes do not register in a shorter period of time. The bone resorption tests can be done more frequently, say, after three months of a therapy, to see if bone breakdown markers are decreasing.
Who Should Get a Bone Density Test?
Anyone with signs or symptoms suggestive of osteoporosis should be tested. Loss of height (indicating spine fractures) or a hip fracture would be examples. Perimenopausal women with risk factors should be tested. The National Osteoporosis Foundation now recommends that all women over age 65 be tested.
Most perimenopausal women have no idea what bone density is or that they are at risk for osteoporosis. I recommend a bone density measurement at menopause, particularly if certain risk factors are present:
- Family history of osteoporosis
- Caucasian or Asian race
- Sedentary lifestyle
- Cigarette smoking
- Moderate to heavy alcohol intake
- Early menopause or hysterectomy
- Poor diet: anorexia, lactose intolerant
Other Causes of Osteoporosis
Sometimes, a specific medical condition or a medication can be causing osteoporosis. If you are found to have low bone density, you need to find out if other treatable factors are contributing. Some endocrine conditions, like hyperthyroidism or hyperparathyroidism, can cause osteoporosis. Severe malnutrition can cause bone loss (called osteomalacia). Some long-term medications, corticosteroids (prednisone), anticonvulsants (taken for seizure disorders), certain diuretics and too much thyroid replacement hormone, can produce osteoporosis. If you must take these medications, there are other medicines that can successfully counteract the bone loss.
How to Treat Osteoporosis
You do not have to jump straight into medication. The truth is that a combination of lifestyle improvements and medication produce the most successful treatment. Currently, there are three key treatment regimens:
- Exercise: weight bearing, weight lifting and balance.
- Nutrition: calcium, vitamin D and protein.
- Medications: ERT (estrogen replacement therapy)/HRT (hormone replacement therapy), raloxifene [Evista®] (a SERM, or Selective Estrogen Receptor Modulator), alendronate [Fosamax®] (a bisphosphonate) and calcitonin [Miacalcin®].
Exercise
Bones respond to stress and weight-bearing exercise, like walking or jogging, and weight training strengthens bones. Balance exercise, like Tai Chi, can also lessen the risk of falls.
Nutrition
A well nourished, well-muscled body is much less at risk for fractures due to falls, even if the bones are weak. Protein is important because the matrix of bone, into which the calcium is inserted, is made of protein. Many women, particularly the elderly, may lack adequate protein intake.
Calcium and Vitamin D are two crucial nutrients for bone formation. Without enough of each, the medicines for osteoporosis don't work as well. Americans, for example, consume a notoriously low calcium diet, estimated at no more than 400-600 mg/day for most adults. The recommended daily intake for mature, menstruating women is 1000 mg/day and for women who are postmenopausal or have had their ovaries removed, 1500 mg/day, the equivalent of three to five servings of dairy products per day. Calcium is also present in green leafy vegetables, canned fish with bones (salmon or sardines), tofu prepared with calcium and orange juice with added calcium.Calcium carbonate supplements contain the highest amount of available calcium (40%) but may not be tolerated by women who are prone to constipation.
It is pretty unrealistic to expect that we can eat enough of these types of food every day, so many women turn to calcium supplements. The first rule about supplements is to identify the calcium-containing compound. It could be calcium carbonate, calcium citrate or calcium gluconate, etc.
Calcium carbonate supplements contain the highest amount of available calcium (40%) but may not be tolerated by women who are prone to constipation. Alternatives are calcium citrate and phosphate. It is important to calculate the amount of elemental calcium available from these supplements, since that is the form of calcium recommended. Sometimes, you need a degree in advanced mathematics or chemistry to figure out how much calcium is contained in each supplement pill. Don't bother trying, just ask your pharmacist. Make sure you are told the number of milligrams of elemental calcium in each pill, not the number of milligrams of calcium carbonate or calcium citrate.
Next, take a look at your daily diet. How much milk, cheese, yogurt, etc., do you eat EVERY DAY? Remember that a serving of dairy yields about 300 mg of calcium. Subtract your daily dietary calcium from your daily requirement (1000 mg premenopausal or 1500 mg postmenopausal). Then plan to take enough calcium in the supplement to make up the difference. If it is calcium carbonate, take it with meals because calcium carbonate is absorbed better with food. If you are taking more than one supplement pill a day, divide the doses among your meals, rather than taking all the supplements with one meal.
Vitamin D is deficient in most American diets. Vitamin D improves the absorption of calcium from the diet. A glass of milk fortified with vitamin D provides 100 IU. For those not eating or drinking enough dairy products, 400-800 IU, the amount in one or two standard multivitamins, is the correct amount. Get out a magnifying glass and read the label.
Medications
ERT (Estrogen Replacement Therapy) & HRT (Hormone Replacement Therapy)
ERT refers to taking estrogen alone; HRT refers to estrogen combined with progesterone. Often the term HRT is used to refer to either regimen, since estrogen is a hormone. Estrogens have been shown to stabilize and substantially reduce the rate of postmenopausal bone loss. For a woman who is perimenopausal, a bone density measurement may help her to make the decision about taking hormone replacement therapy. If bone mineral density is low, HRT will address the issue of preserving bone as well as other perimenopausal medical problems, like the increased risk of heart disease. Women who have an intact uterus should take cyclical therapy (estrogen 25 days, progesterone 10 days) or combination therapy with progesterone (estrogen and progesterone every day) to eliminate the risk of uterine cancer. If you have had previous breast cancer, you should not take HRT.
Despite the benefits of estrogen, many women are reluctant to take it for fear they may develop breast cancer. Most authorities now think there is a slight increase in risk after years of treatment with estrogen. Another problem with HRT is uterine bleeding, which can be quite heavy with cyclical therapy and unpredictable with combination therapy. Many women, up to 40% percent in some studies, who started HRT discontinue it, often without follow-up or continuing therapy with another regimen.
Deciding about HRT
A woman's decision has to be based on a balance of many factors. She has to look at her own risks for osteoporosis, coronary heart disease, breast cancer and urinary/genital symptoms and decide. The decision should be based on firm medical evidence about her risks and benefits. When it comes to osteoporosis, estrogen is the best treatment we have for building and maintaining bone.
One thing I would like to say is the if you decide to take ERT/HRT, DO IT! Fill the prescription, take the medicine and give yourself enough time to see what the side effects and beneficial effects are. If you want to stop or change, consult with your doctor and try something else. The reasons you decided to go on HRT have not changed. You owe it to yourself and your bones, heart, etc., to continue taking responsibility for preventing future illness.
SERMs (Selective Estrogen Receptor Modulators)
Estrogen affects many tissues in the body. It does so by attaching to receptors on different types of tissues. A number of years ago investigators discovered that by modifying the structure of estrogen, the resulting compound would either imitate or block the estrogenic effect on specific tissues. This is the basis for the class of medicines known as selective estrogen receptor modulators (SERMs).
Tamoxifen
The most well-known SERM is tamoxifen (Nolvadex®), which is used in the treatment of breast cancer. Tamoxifen blocks the effect of estrogen on breast tissue and has been shown to decrease recurrence and new tumors in women who have had breast cancer. Tamoxifen has also been given to women at high risk for breast cancer and has been found to decrease the rate of breast cancer development. One drawback to tamoxifen is that it retains the stimulatory effect of estrogen on the uterus and may be responsible for polyps and even cancer of the uterus.
Tamoxifen has an interesting effect on bone. In postmenopausal women, it acts like estrogen, stabilizing and increasing bone density. In premenopausal women, tamoxifen decreases bone density, probably because it gets in the way of natural estrogen. A premenopausal woman with low bone density, who is taking tamoxifen for breast cancer prevention, should also be on a bone-building drug like alendronate to counteract the premenopausal tamoxifen effect.
Raloxifene (Evista®)
Raloxifene, another SERM, was released in 1997 and is specifically indicated for postmenopausal osteoporosis. Its advantage is that it has no stimulatory effect on either breast or uterine tissue. There is not yet enough proof to say that raloxifene has the same beneficial effects on heart disease as estrogen but studies are currently going on to test this effect. Raloxifene is also being investigated to see if it will reduce the risk of breast cancer.
One disadvantage in postmenopausal women is that the SERMs do not reduce the hot flashes of menopause and may, in some cases, increase them.
Alendronate (Fosamax®)
Alendronate (Fosamax®), a member of the class of medicines known as biophosphonates, was released in 1996 for the treatment of osteoporosis. At a 10 mg daily dose, it also works by decreasing bone resorption and can be used as an alternative in women unable to take estrogen. Alendronate can be used in addition to estrogen in women with severe disease. Its absorption characteristics make alendronate somewhat awkward to take but once these are mastered this compound has been shown to be very effective. Alendronate is very poorly absorbed and must be taken with a full glass of water on an empty stomach that will remain empty for at least 1/2 hour, usually first thing in the morning. Maintaining an upright posture at this time is also recommended because of the development of lower esophageal erosions in some cases. Adequate calcium (1000-1500 mg) and vitamin D (400-800 IU) must also be taken daily to support the net bone build-up.
Calcitonin
Calcitonin is a hormone that can halt bone resorption. Available for a number of years in a subcutaneous or intramuscular injected form, it now exists as an intranasal preparation of calcitonin (Miacalcin®). One spray into a single nostril daily, alternating sides, provides a 200 mcg dose, which, when absorbed, is as effective as the 100 mcg subcutaneous dose. Calcitonin has been shown to be more effective on the BMD of the spine than of the hip. One remarkable thing about calcitonin is that it has an analgesic effect on fractured bone, especially on painful spine fractures. Because of calcitonin's strong antiresorptive effect that results in increased bone formation, adequate vitamin D (400-800 IU) and calcium (1000 mg) must be taken daily with this drug. The main side effect, not surprisingly, is nasal irritation and dryness. There is some concern about adequacy of absorption in the presence of an upper respiratory infection.
Summary
The "dowager's hump" and the fractured hips of osteoporosis are not an inevitable consequence of aging. You can take steps throughout your lifetime to build up and maintain a strong skeleton. You can have a bone density test to find out exactly how strong your bones are. There are many lifestyle changes and pharmaceutical options to help you maintain or regain healthy bones.ADVERTISEMENT