People tend to use the word insomnia casually, but insomnia is more than just occasional tossing and turning in bed. It is a debilitating, often chronic illness. To be diagnosed with true insomnia, you must have a problem falling asleep, staying asleep or getting enough rest from sleep that interferes with work or other everyday tasks. People with insomnia often find it difficult simply to get through the day.
Six of the ten most frequently prescribed insomnia drugs have never actually been studied for this use; the most frequently administered drug has been the subject of a single study, which, incidentally, suggested that it did not work.
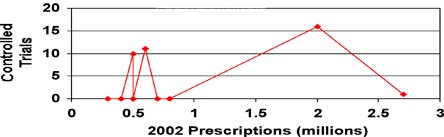
Figure 1 shows that a drug that was prescribed 2.75 million times in 2002 had been studied only once; between 0.5 and 1 million prescriptions of two other drugs were written without any study having been carried out; between 0.25 and 0.5 million prescriptions were written for three others, also without a single study supporting their use for insomnia.
- Chronic insomnia interferes with the ability to work and to perform ordinary daily tasks.
- Insomnia needs to be treated directly, even when it co-exists with serious medical and psychiatric conditions.
- There are effective non-drug therapies.
- Treating insomnia along with a related psychiatric or medical condition is not only possible, but can even improve the related condition.
Obviously, many people without insomnia experience these symptoms from time to time. It is the severity of these symptoms and how much they interfere with a person's life and functioning that determines whether or not treatment for insomnia is needed. If you experience some or all of these in association with difficulty with your sleep and feel that they interfere with your daily functioning or quality of life, you should see your doctor or other medical practitioner.
The latest research suggests that insomnia needs to be treated directly, even when it occurs together with other medical and psychiatric disorders.
The conventional idea was wrong. The latest research suggests that insomnia needs to be treated directly, even when it occurs together with other medical and psychiatric disorders.13,14,15 The severity of insomnia can not only make a medical or psychiatric illness worse, buy it can actually serve as a sort of barometer that helps predict adverse outcomes and future episodes of both medical and psychiatric problems. In 2005, a NIH (National Institutes of Health) State-of-the-Science Conference panel urged doctors to consider new evidence (see below) that treating insomnia may also improve many associated conditions.
When doctors decide which treatment to recommend, they look to the scientific data for answers. Unfortunately, insomnia data are very meager for certain subgroups. In children and the elderly, for example, the risks of some insomnia drugs are likely greater than or different from the those for adults aged 21-65, who have been the focus of the vast majority of insomnia drug trials. In fact, there has yet to be a single published study of any drug for insomnia in children.
The same is true for those with medical and psychiatric conditions such as major depression, anxiety disorders, chronic pain, etc. Response to treatment and vulnerability to side effects probably vary quite a bit within this group. While solid data on many diseases have been lacking, specific studies have recently been done on the treatment of insomnia along with depression, generalized anxiety disorder, rheumatoid arthritis and fibromyalgia (See Table 5).
In one large study of insomnia occurring along with major depressive disorder (MDD), some subjects treated with fluoxetine for their depression were also treated for insomnia with the drug eszopiclone. Those given eszopiclone not only slept better but also had a faster and better response to the antidepressant.
| Caffeine | Limit use. Eliminate evening/night intake |
| Alcohol | Limit use. Eliminate evening/night intake |
| Nicotine | Eliminate smoking at night |
| Exercise | Eliminate exercising close to bedtime |
| Food/Liquid intake | Eliminate excessive intake close to bedtime but encourage eating enough not to promote waking up due to hunger |
| Light | Maintain a dark bedroom at night |
| Noise | Eliminate noise in the sleep environment |
| Temperature | Maintain comfortable temperature in bedroom |
- Progressive Muscle Relaxation
- Biofeedback
- Hypnosis
- Guided Imagery
- Meditation
- Get out of bed when unable to sleep, or when frustrated or anxious about sleep
- Do not worry, think or plan in bed
- Go to bed only when tired to the point where sleep seems inevitable
- Use the bed only for sleep and sex (no reading or watching TV)
In choosing to go the non-drug route, the most important considerations are your willingness and ability to commit to changing longstanding behaviors. Behavioral changes can be daunting, in the same way that eating less to lose weight is extraordinarily difficult for some people. Without a high level of motivation, behavioral therapies are doomed to fail. Furthermore, some insomniacs simply cannot carry out the required behavior changes. This includes those with medical illnesses that keep them bed-ridden and those with disorders such as severe major depression, dementia, mental retardation and schizophrenia.
Lastly, it is only in a subset of cases that behavior perpetuates insomnia. For those without behavioral perpetuating factors, cognitive and behavioral interventions are very unlikely to treat insomnia effectively.
Recently, a new drug, ramelteon, became available for insomnia. Other antidepressants used to treat insomnia include amitriptyline, doxepin, tri-imipramine, mirtazapine, nefazodone and trazodone. Antipsychotics can also enhance sleep; those most commonly used to treat insomnia are quetiapine and olanzapine. Anti-histamines are the most commonly used over-the-counter sleep aides.
In deciding which of these is right for you, it is necessary to discuss with your doctor whether a particular drug has been shown to be effective for the type of insomnia you are experiencing. As discussed above, only the FDA approved drugs (benzodiazepines, melatonin receptor agonists and non-benzodiazepines) are backed by hard science. Table 5 lists the drugs that have been proven effective in treating insomnia.
| Agent | Sleep Onset | Sleep Maintenance | Longest Controlled Trial | Older Adults |
|---|---|---|---|---|
| Benzodiazepines | ||||
| Triazolam 0.25 mg | + | 4 Weeks | + | |
| Triazolam 0.5 mg | + | + | 2 Weeks | + |
| Flurazepam 30 mg | + | + | 4 Weeks | + (15-30 mg) |
| Estazolam 1/2 mg | + | + | 2 Weeks | |
| Quazepam 30 mg | + | + | 2 Weeks | |
| Temazepam 30 mg | + | + | 8 Weeks | + (7.5-30 mg) |
| Non-Benzodiazepines | ||||
| Zolpidem 10 mg | + | 5 Weeks* | + (5 mg) | |
| Zolpidem CR 12.5 mg | + | + | 3 Weeks | |
| Zaleplon 10 mg | + | 5 Weeks | + (5-10 mg) | |
| Eszopiclone 2/3 mg | + | + | 6 Months | + (2 mg) |
| Melatonin Receptor Agonists | ||||
| Ramelteon 4-32 mg | + | 5 Weeks | + | |
| Antidepressants | ||||
| Doxepin 25-50 mg | + | + | 4 Weeks | |
Table 5 lists therapies (both drug and non-drug) that are proven effective for insomnia when it occurs with another condition.
As with all drugs, side effects are listed on the FDA approved label. Given the same dosage of medication, there is a greater likelihood of side effects in older adults. Principal side effects of benzodiazepines and non-benzodiazepines are sedation, dizziness, amnesia and ataxia (clumsiness). Antidepressants and antipsychotics can cause sedation, dizziness and low blood pressure. Over-the-counter sleep medicines can cause daytime sedation and dizziness.
Once drug therapy is begun, there is no easy way of determining when the insomnia has been cured. As a result, it is necessary — typically every 2-3 months — to try stopping the drugs.
Another crucial part of follow-up is to the decision to stop therapy. We currently have no way of determining how long a particular case of insomnia is likely to last. Also, once drug therapy is begun, there is no easy way of determining when the insomnia has been cured. As a result, it is necessary — typically every 2-3 months — to try stopping the drugs. This should be done with a very gradual tapering off and only under a doctor's supervision.
As seen in Table 5, only a few anti-insomnia drugs have been proven effective for periods of over one month and only one has been evaluated as long as six months. However, studies have shown that for some medications dependence is unlikely and that treatment, even as long as six months or more, can be safe and effective.




