Dr. Pandol is Professor of Medicine, UCLA School of Medicine and Staff Physician, Department of Medicine, VA Greater Los Angeles Health Care System and University of California, Los Angeles.
The pancreas is an important gland located near the stomach and the small intestine which makes a variety of key chemicals ("enzymes") that help regulate different bodily processes. The pancreas secretes enzymes into the small intestine that help us digest food, and it also produces and then releases the hormones insulin and glucagon into the bloodstream to control the level of sugar (glucose). Sometimes the enzymes become active while they are still inside the pancreas. When this happens, they damage the pancreas itself.
In a healthy person, digestive enzymes produced by the pancreas are activated when they reach the small intestine. Sometimes, however, the enzymes become active while they are still inside the pancreas. When this happens, they damage the pancreas itself ("pancreatitis") and cause a variety of other problems.There are two kinds of pancreatitis: acute and chronic. Acute pancreatitis happens in sudden, brief attacks,while chronic pancreatitis lasts longer and causes a slow but steady destruction of the pancreas. Both can cause other serious problems such as bleeding, damage to the heart and other organs, and infection.
The most common first symptom is abdominal pain, often accompanied by vomiting, fever, tachycardia (racing of the heart), high white blood cell count and increased levels of pancreatic enzymes in the blood and urine. In severe cases, acute pancreatitis affects other organs, (e.g., lungs, kidneys, liver, the cardiovascular and central nervous systems).
Acute pancreatitis can be further subdivided into mild and severe: in the mild form, the disease causes little organ dysfunction and the body recovers more or less on its own; in the severe form, the disease causes multiple organ failure, tissue death, abscesses and pseudocysts. Pseudocysts are discussed below.
There is uncertainty as well about how common acute pancreatitis really is. Estimates range from 5 people per 100,000 all the way up to 73 per 100,000. The reason for this is that pancreatitis is easy to miss or misdiagnose. Also, many people do not seek medical attention because their symptoms are mild or because of limited access to medical care.
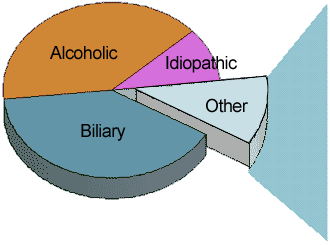
Alcohol abuse is more commonly associated with male cases than female cases, whereas gallstone disease is more commonly associated with female cases. For this reason, the total number of acute pancreatitis cases, and the disease's distribution by sex, in different areas of the world have a lot to do with local alcohol customs and the prevalence of gallstones.
Where there are symptoms and signs of acute pancreatitis, tests such as measures of serum enzymes and pancreatic imaging studies (i.e., ultrasound, CT) are needed to establish the diagnosis. Table 1 presents an overview of the diagnostic tests.
| Test | Sensitivity | Specificity | Comment |
|---|---|---|---|
| Serum enzymes | high | moderate | > 3x normal increases specificity |
| Ultrasound | moderate | high | Best for gallstones |
| CT | moderate | high | Detects calcifications, fluid collections |
| CT with pancreatic protocol and IV contrast | moderate | high | Detects necrosis |
Often, contributing factors for someone with an episode of acute pancreatitis cannot be identified right away. In this case, imaging techniques are used. Autoimmune pancreatitis can be diagnosed by imaging and other tests, while the genetic causes require formal genetic testing.
- Autoimmune
- Drug induced
- Iatrogenic
- IBD related
- Infections
- Inherited
- Metabolic
- Neoplastic
- Structural
- Toxic
- Traumatic
- Vascular
Early assessment of severity is critical for identifying those who require intensive monitoring and support.
A practical approach to determining severity is to monitor the indicators listed in Table 2, together with other tests.
- Tachycardia, hypotension
- Tachypnea, hypoxemia
- Hemo-concentration
- Oliguria
- Encephalopathy
| Supportive Car | Other Treatments |
|---|---|
|
|
If imaging studies show gall bladder obstruction and infection caused by gallstones, doctors may recommend immediate surgery to remove the gallstone or stones.
In those who have signs of pancreatic infection (pseudocysts or abcesses), the suspicious pancreatic lesion should be tested for infection. Lesions found to be infected can be removed or destroyed using radiology or surgery. Antibiotics may also be used.For those with severe pancreatitis, preventive antibiotic therapy can be particularly effective. However, not all medical experts agree about this.
A recent study showed that preventive antibiotics reduced mortality, but the advantage was limited to those with severe acute pancreatitis who received so-called broad-spectrum antibiotics that fight a wide variety of bacteria. The largest Randomized Control Trial compared a combination of two agents as against a placebo (ciprofloxacin + metronidazole vs. placebo) involving 114 people showed no benefit. Antibiotics used in acute pancreatitis include imipenim alone; cefurozime alone; ceftazidime, amikacin and metronidazole; and ciprofloxacin and metronidazole.
Better choices for pain management are hydromorphone, fentanyl and morphine. It is important to be careful with these medicines, because all narcotics cause depression of respiratory and cardiovascular functions, which can be made worse by other drugs used in acute pancreatities cases such as calcium channel blockers and beta-adrenergic antagonists.
Those with severe pancreatitis, whose symptoms last more than 5 days, are often given a feeding tube.
Pseudocysts are collections of pancreatic fluid contained by scar tissue. The fluid contains high concentrations of pancreatic enzymes. Pseudocysts are common, appearing in up to 10% of those with acute pancreatitis. They may cause upper abdominal pain, a full feeling, nausea and vomiting. Pseudocysts sometimes rupture and leak pancreatic fluid into the abdominal cavity.
Most pseudocysts go away by themselves and are only drained when there is evidence of infection or when the pseudocyst continues to enlarge.
Pancreatitis has two forms: acute and chronic
Many cases of pancreatitis appear to be caused by gallstones or alcohol abuse.
In some cases, there is no clear cause.
Symptoms include abdominal pain, nausea, vomiting, fever and a rapid pulse.
Treatments include pain killing narcotics, IV fluids, antibiotics and surgery.




