"Modern cardiology has given up on curing heart disease." -- Caldwell B. Esselstyn, M.D.
This is a shocking statement considering the impressive array of treatments available to today's cardiologists.
With coronary artery bypass surgery, balloon angioplasty and stent implantation, plus many sophisticated high-tech tests, the odds would seem to favor 21st century heart patients.But not only are all of these techniques aggressive and expensive, the real problem is they don't work. They don't correct the causes of heart disease. They don't stop the processes that create atherosclerosis (narrowing of the arteries) and, in most cases, they don't help people live longer since the basic causes persist.
There is, however, an alternative called reversal therapy. Conventional treatments focus on the symptoms of heart disease, such as chest pain due to narrowing of the arteries. But this narrowing is the end product of a long, complex process of cholesterol accumulation in the wall of the artery. Even before significant narrowing occurs or symptoms, the cholesterol plaque may break or rupture and cause a clot or thrombosis in the coronary artery. This clot blocks blood flow to the heart and leads to a heart attack, sudden chest pain and stroke despite no previous warning signs. Reversal therapy is different. It treats the underlying causes of cholesterol accumulation and plaque rupture such as high cholesterol levels, smoking, excess weight, an unhealthy diet, lack of exercise, high blood pressure, diabetes and stress.
Atherosclerosis is the process of cholesterol accumulation, along with inflammation, scarring and calcification (hardening) of the coronary arteries, which lead to plaque rupture and heart attack or narrowing that causes chest pain.
Conservative estimates suggest that 20% to 40% of middle aged people in the United States today have early coronary atherosclerosis or silent heart disease. Unfortunately, the way many of them find out is by having a heart attack. Statistically, as many as 60% to 85% of heart attacks and sudden deaths from heart disease occur without any warning from rupture of the cholesterol plaque without previous narrowing. Most victims never knew they were at risk and never sought any kind of treatment. Chest pain and other symptoms that send people to the doctor tend to be caused by slowly developing severe or partial blockage of the arteries. In contrast, most heart attacks happen suddenly without warning in people whose atherosclerosis has not caused slow or partial narrowing but rather sudden complete blockage because of rupture of the cholesterol plaque where there was no significant narrowing previously.
The reason for this is that, while narrowing of the arteries is clearly related to heart attack risk, there are other factors at work. Atherosclerosis works like this: a pool of lipids, or fat collects in the wall of the artery. The body reacts by covering these plaques with a cap made up by the lining of the arterial wall. The cholesterol also causes inflamation and scarring of the wall — bumps or patches made up mostly of scar issue — and covering these in turn with a new lining. As scar tissue builds up, these plaques grow and narrow the artery, interfering more and more with the flow of blood. At some point, the decreased blood flow to the heart may cause chest pain, shortness of breath or another symptom that will bring you the doctor's office. Well before that point, however, one or more plaques may rupture, or break away from the arterial wall, and form a sudden, complete blockage of blood flow. This causes a type of heart attack, also called myocardial infarction.
Unfortunately, these factors are not related to each other and none is directly related to the severity of the arterial narrowing. This explains the unpredictability and seeming randomness of this type of heart attack.5 Research has shown that most cases of plaque rupture happen to people whose arteries are only slightly or moderately narrowed and who have no symptoms. In fact, these apparently healthy people are actually at greater risk for heart attack than those with symptoms because younger, smaller plaques with more fat and less scar tissue rupture more easily than the older, more scarred plaques that cause more severe arterial narrowing.
The standard test that most cardiologists use to detect coronary heart disease is coronary arteriography, also known as arteriogram or angiogram. While this test is good at measuring the degree of narrowing in a particular section of artery, there are a number of important factors that it does not measure, including the likelihood that plaque rupture will take place.7 Moreover, arteriography cannot measure the cumulative damage that coronary atherosclerosis causes throughout the entire circulatory system.
The 3-D PET test is used as the basis for reversal therapy. It is non-invasive and involves only an intravenous injection. PET can detect the build-up of lipids throughout the arteries long before severe narrowing occurs. Compared to arteriography, PET more accurately indicates the diffuse cholesterol buildup along the whole length of the coronary artery rather than just narrowing in a specific section of artery. In reversal therapy, PET tests are used both for diagnosis and to monitor the heart patient's progress through and beyond treatment.
In a word, the answer is yes.
Recent studies of people who were put on a vigorous cholesterol-lowering program, using a moderate low fat diet and cholesterol-lowering drugs, as well as others who were put on a very low-fat diet without drugs, showed that as many as 85% saw their heart disease either stop progressing or begin to reverse. People on these diets also saw improvements in the degree of arterial narrowing; the improvement was a small, but consistent, turnaround of 3% to 10%. Most importantly, there was a major decrease in the likelihood that they would experience heart attack, death, bypass surgery or balloon angioplasty. Other studies around the world have confirmed these results.
All these studies have further underlined the importance of diet by showing that high fat food raises their risk of developing coronary heart disease separately from blood cholesterol levels. For example, in one study, a group of people following the American Heart Association dietary guidelines — eating 20% of overall calories as fat — showed no change over time in the progression of their coronary artery disease or in their risk of having a heart attack. When their fat intake was lowered to 10%, their heart disease either stopped or began to regress. Their risk of having a heart attack also went down
.The bottom line is that while people with high cholesterol numbers are clearly more likely to have heart disease or a heart attack, high dietary fat is also a strong risk factor separately from blood cholesterol levels.
In the author's experience, the combination of a very low fat diet and the use of a combination of lipid-reducing and anti-cholesterol drugs can lower a person's risk of heart attack by 90% or more. Even better, there does not seem to be a down side. Studies have shown that very low cholesterol levels and very low fat diets do not cause any increase in the risk of death from other causes. In fact the opposite occurs; in patients with coronary artery disease and relatively normal cholesterol, lowering cholesterol to well below normal ranges has substantial health benefits. Weight control by reducing carbohydrate calories is also important but often overlooked in the focus on reducing dietary fat.
There is no question that vigorous cholesterol lowering through a low-fat, low carbohydrate diet and cholesterol lowering drugs can dramatically improve coronary and arterial health in as little as 90 days. This is confirmed by using PET scans that measure the efficiency of overall blood flow throughout the arteries. The medical term for this is myocardial perfusion.
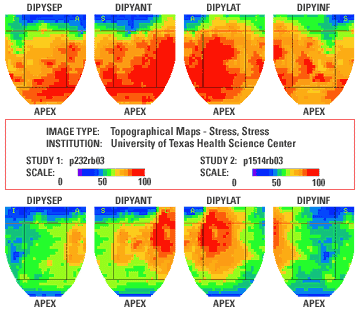
In Figure 1 above, we show the beginning (or baseline) PET scan in the top row. The color scale relates to blood flow. Red and yellow indicate high blood flow to the heart, while green, blue and black indicate much lower blood flow. The bottom row, taken five years later in a patient who has not had treatment, shows definite worsening throughout the heart — the red and yellow colors areas are now mostly green and blue.20
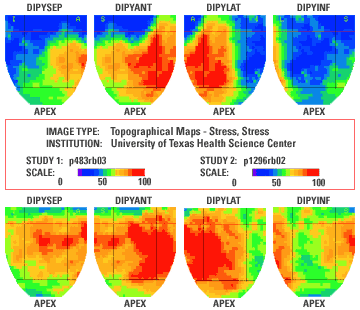
Figure 2 shows an example of PET at baseline (upper row) and after five years of lifestyle change (lower row) with the same views and color scale. Blood flow in the heart has dramatically improved.
Most people who seek treatment for coronary heart disease will be offered a range of surgical procedures (revascularization) to bypass the blocked arteries. These commonly include coronary bypass and balloon angioplasty. These procedures have been done frequently enough and long enough that today there is little doubt about whether or nor they are effective in changing the course of the disease. They are not. Long-term follow-up studies of people who underwent coronary bypass surgery — but did not address diet or cholesterol levels — show little or no decrease in their overall risk of heart attack (myocardial infarction) or death. In a similar study involving bypass surgery, angioplasty and other conventional treatments targeting specific areas of arterial narrowing, after three years there was no difference in reduction in the risk of heart attack or death, or the incidence of chest pain.
A comparison of several major coronary bypass studies found that lowering cholesterol alone was a far more effective treatment than either bypass surgery or angina-reducing drugs on improving long term survival. In the large number of patients whose primary health problem is coronary heart disease, the prevailing philosophy of using surgical procedures as a primary treatment does not lengthen and may even shorten life, whereas cholesterol lowering dramatically reduces the risk of heart attack and prolongs life. On the other hand, certain types of patients with severe involvement of all coronary arteries and impaired heart pumping function clearly show improved survival after bypass surgery of balloon dilation.
What explains the ineffectiveness of these surgical procedures? The answer is simple — they do not alter the basic disease process occurring throughout the coronary artery. In the absence of a vigorous reversal program, bypass surgery, balloon angioplasty and stenting will not prevent plaque rupture and heart attack. Since revascularization procedures do not reduce risk of heart attack from myocardial infarction or mortality in patients with otherwise healthy hearts, the rationale frequently given by doctors for a revascularization procedure, "to prevent a heart attack or dying," is fundamentally false. All of our best information indicates that the best treatment for preventing heart attack and death due to coronary artery disease is reversal treatment centered around vigorous cholesterol lowering.
Reversal therapy consists of early detection using PET scans, followed up by a regimen, tailored to the individual by his doctor, of cholesterol-lowering drugs, low-fat diet, weight control by reduction of carbohydrate calories, exercise, stress management and quitting smoking. It is an effective alternative to revascularization procedures in most patients. In this noninvasive approach, PET takes the place of standard stress testing and coronary arteriography, while vigorous risk factor treatment replaces angioplasty and bypass surgery except for a small proportion of patients that do need these procedures. This approach is safer, far less expensive and more effective than conventional, more invasive treatments.