Professor of Medicine, University of Chicago School of Medicine, Chicago, IL.
Few of us take it seriously. Many of us even brag about not getting enough. We are talking about sleep.
Sleep — or the lack of it — is not usually thought of as an important health issue, but it certainly can be when we do not get enough for long enough. The occasional all-nighter is no big deal, but long-term sleep loss can cause or contribute to a wide range of physical and psychological problems, which is why sleep deprivation is used as an interrogation tool and has been a topic in recent policy debate in the United States over the definition of torture.
Adequate sleep has long been considered to be important for the brain but not for the rest of the body. Now, there is growing evidence that sleep loss or poor quality sleep may increase the risk of obesity and diabetes, as well as compromising the immune system.
Sleep Loss and Modern Times
Modern society often views sleep loss as harmless or even as a sign that someone is hard-working and efficient. The increasing demands of many jobs and our around-the-clock access to leisure and work have also shortened sleep times. In industrialized societies, roughly 20% of the work force is engaged in shift and other work schedules that tend to lead to substantial sleep loss. People lose sleep for a variety of reasons. Sleep loss can occur simply because we choose to go to bed late and get up early, or because of a physical or psychological problem. Whatever the cause, sleep loss is increasingly common in modern society.
This did not happen overnight. In 1960 the average person got 8.0-8.9 hours of sleep per night. By 2002 the average American slept 6.9-7.0 hours. In 2004, more than 30% of adult men and women between the ages of 30 and 64 years reported sleeping fewer than 6 hours per night. And a recent study evaluating sleep duration using an electronic device rather than self-reporting found the average to be 6.1 hours.Now, there is growing evidence that sleep loss or poor quality sleep may increase the risk of obesity and diabetes, as well as compromising the immune system.
Children and adolescents are no exception; and for them, the stakes are higher. Adolescents need for sleep has been estimated to be around 9 hours. But they only get about 6.9 hours a night as 12th graders, decreasing steadily from 8.4 hours as 6th graders. A surprising 28% of high school students admitted falling asleep at school at least once a week.
The effects of all this sleep loss may be far more serious than simply being tired. The dramatic increase in obesity and diabetes has occurred at the same time as this decrease in sleep. The two trends mirror each other over the second half of the 20th century. Is one causing the other? It is too soon to say, but the association between the two phenomena is undeniable.
Sometimes, chronic sleep loss is a known symptom of a number of conditions, including insomnia and obstructive sleep apnea (OSA) in which people stop breathing repeatedly during their sleep, often for a minute or longer and up to hundreds of times during a single night. Insomnia becomes more common with age. Today, with the aging of the U.S. population, chronic insomnia is estimated to affect 10-15% of the public population. In middle-aged adults, OSA affects about 24% of men and 9% of women. Data from the 2005 Sleep in America poll by the National Sleep Foundation indicate that as many as one in four adults, and more than 50% of obese adults, are at high risk for OSA. While OSA causes sleep fragmentation, respiratory disturbances and hypoxic stress (low levels of oxygen in the body) along with sleep loss per se, reduced total sleep time is a common symptom.
Taken together, sleep loss, either behavioral or disease-related, affects millions of individuals in our modern society. Recent laboratory and epidemiologic studies indicate that sleep loss may damage your health. These studies have focused on sleep deprivation's role in:
- blood glucose levels and diabetes risk
- appetite regulation and obesity risk
- immune function.
Sleep Loss and Diabetes
The body's glucose regulation mechanism operates quite differently during sleep than in waking hours.10 Blood levels of glucose are tightly regulated by the body and kept within a narrow range to avoid both hypoglycemia (low blood sugar) and hyperglycemia (high blood sugar). Both conditions have serious, even life-threatening consequences.
An early study looked at glucose tolerance in healthy young men who were subjected to 6 nights of 4 hours in bed ("sleep debt") followed by 7 nights of 12 hours in bed ("sleep recovery"). At the end of each bedtime session, the subjects underwent an intravenous glucose tolerance test (ivGTT) and a 24-hour period of frequent blood sampling.
The amount of insulin released following glucose injection, referred to as the "acute insulin response to glucose," was 30% lower when the subjects were in a state of sleep debt than when they were fully rested. Taken together, the findings indicated that glucose metabolism in these young adults after less than one week of sleep restriction was similar to that of older adults with impaired glucose tolerance, i.e., in a pre-diabetic state. The findings of this first "sleep debt" study were confirmed by a second study that examined the impact of sleep restriction (4 hours per night for 2 nights) and sleep extension (10 hours per night for 2 nights).Glucose metabolism in these young adults after less than one week of sleep restriction was similar to that of older adults with impaired glucose tolerance, i.e., in a pre-diabetic state.
Several later studies on the possible link between diabetes and sleep loss using subjects' self-reports of sleep times found a significant association between sleep loss and the risk of developing Type 2 diabetes. Seven studies, from Germany, Japan, Sweden and the U.S., have been published so far.
The possibility that there could be an association between short sleep duration and diabetes was addressed in another recent study. Self-reported sleep duration, sleep quality and hemoglobin A1c levels, a key marker of glucose control, were examined in African Americans with Type 2 diabetes. Perceived sleep debt was calculated as the difference between preferred and actual sleep duration. After controlling for age, gender, BMI and insulin use, it was found that levels of hemoglobin A1c were associated with perceived sleep debt. The effect of getting more sleep was comparable to that of widely used oral anti-diabetic drugs. While these associations suggest that improving sleep duration or quality for those with Type 2 diabetes may improve glycemic control, they do not prove that sleep loss directly causes diabetes.
The mechanisms underlying changes in glucose metabolism following long-term sleep loss are complex. Sleep loss has been linked to decreased brain glucose metabolism, increased sympathetic nervous activity, elevated levels of evening cortisol, increased secretion of ghrelin and growth hormone during waking hours and increased levels of pro-inflammatory cytokines. All of these factors are known to interfere with the body's ability to regulate glucose.
Sleep Less, Eat More...and More
Our appetite is regulated by hormonal signals. These hormones include leptin, which creates a feeling of fullness and satisfaction, and ghrelin, an appetite-stimulator. Leptin informs the brain of the status of energy stores in fat tissue. Low energy stores and low leptin levels cause us to eat more. Ghrelin is released primarily from the stomach. Studies indicate that ghrelin is partly responsible for mealtime hunger and meal initiation. Ghrelin levels drop rapidly after we eat, then rebound after 1.5-2 hours, paralleling a return of hunger. Leptin and ghrelin exert opposing effects and have been referred to as the "yin and yang" of appetite regulation.
Sleeping and eating are fundamentally related. At the risk of stating the obvious, being awake is required for feeding and sleep requires fasting. Sleep deprivation in animals occurs mainly when there is a shortage of food and extended wakefulness is needed for foraging. Homo Sapiens may well be the only mammalian species that voluntarily deprives itself of sleep in the absence of an emergency.Sleep loss in humans causes a loss of control over appetite, promoting a kind of false hunger, unrelated to actual need.
In animal models, sleep loss causes increased appetite, as well as considerable stress. Rodents submitted to sleep deprivation for long periods of time increase their food intake It is not known whether sleep loss in humans under comfortable conditions, e.g., in an armchair in front of a television, has similar effects.
Sleep loss in humans causes a loss of control over appetite, promoting a kind of false hunger, unrelated to actual need. Leptin concentrations were much lower at the end of sleep restriction than at the end of the recovery period. Leptin levels appear to be very sensitive to sleep duration; reducing sleep duration by as little as 2 hours lowers the levels of this satiety ("fullness") signal.
Sleep Loss and Hormone Levels
The effect a lack of sleep has on appetite seems to be related to the hunger-promoting hormone, ghrelin. One study found that as levels of leptin decreased by 18% during periods of sleep restriction, the levels of ghrelin, increased by 28%.
The study subjects' own ratings of their hunger and appetite levels were higher during sleep restriction than sleep extension. When they did not get enough sleep, the subjects reported craving carbohydrate-rich foods (+32%) more than other foods (+18%), possibly because the "tired" brain craves glucose, its major fuel.
How long you sleep can affect appetite as well. Short sleep is associated with higher morning ghrelin levels and lower leptin levels. Sleep loss may alter the ability of leptin and ghrelin to accurately signal caloric need, acting in concert to "fool" the body into thinking that it needs more energy.
Thirteen epidemiologic studies in adults and 8 in children have reported that sleep loss is associated with increased BMI. This association was observed in studies that enrolled subjects with different BMI, from lean or mildly overweight to obese, and from different countries and cultures. While the evidence for an association between sleep loss and obesity is rapidly building, it should be noted that nearly all studies have relied on subjective reports of sleep duration.
Taken together, the evidence from laboratory and epidemiologic studies raises the possibility that chronic sleep loss, a novel condition that seems to have become widespread in modern societies and particularly in the U.S., may play a role in the current epidemic of obesity. An increasing "sleep debt" has been considered as the number one non-traditional explanation for the epidemic of obesity, after the traditional causes — excessive caloric intake and decreased physical activity. Many recent studies suggest that sleep loss may in fact cause excessive food intake. This, however, is far from proven.
Sleep Loss and the Immune System
Adequate sleep is important for immune function. Sleep deprivation elevates levels of inflammatory markers such as interleukin-6, tumor necrosis factor and C-reactive protein suggest that the risk or severity of many medical conditions that involve chronic inflammation (e.g., cardiovascular disease, diabetes, arthritis) could be increased by sleep loss.
Sleep also seems to play an important role in efficient immune defense; the popular wisdom that not getting enough sleep increases your chances of catching a cold may well be true. One study examined the antibody response to hepatitis A vaccination over a 28-day period in healthy young subjects who either had a normal night of sleep following inoculation or were kept awake all night.33 Post-vaccination antibody levels were nearly 50% lower in those who had been sleep deprived, compared to those who had a normal night's sleep. Another study examined the response to influenza vaccination after 4 consecutive nights of partial sleep deprivation (only 4 hours per night) and continued bedtime restriction for 2 more nights, as compared to immunization preceded and followed by normal amounts of sleep.34 Figure 1 illustrates the findings.
Figure 1.
Antibody Titers in Sleep Deprived and Normal Sleep Subjects.
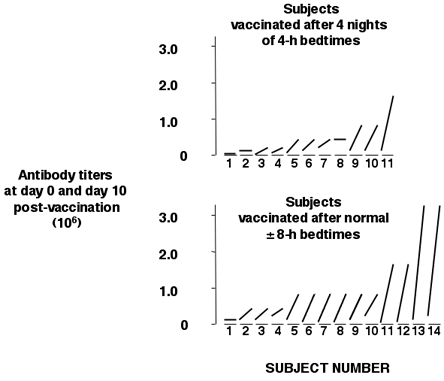
On average, antibody titers on the 10th day after immunization in those who had been sleep-deprived were half those of subjects with normal sleep. The two studies support the idea that sleep loss interferes with immune response. They also suggest that prior sleep history should possibly be considered when people are undergoing vaccination. It is also possible that some of the well-documented effects of stress on immune function could be aggravated by sleep loss and that the loss of sleep time and quality that come with aging may explain why vaccines are not as effective in the elderly.
Conclusions
Clearly, adequate sleep is essential, not only for the brain but also for the rest of the body. Recent studies suggest that sleep loss, a very common condition in modern society, could be a risk factor for several major chronic diseases, including obesity and diabetes.
ADVERTISEMENT




