Amblyopia, or “lazy eye,” is the most common cause of single eye visual impairment for children and young adults. Amblyopia occurs when normal eyesight in one eye is disrupted during a critical period in visual development. This leads to a unilateral (one-sided) or, less commonly, bilateral (both-sided) decline in best-corrected visual acuity (BCVA) – the best vision one can achieve even when they are using proper glasses or contact lenses.
Amblyopia occurs when normal eyesight in one eye is disrupted during a critical period in visual development.
The decreased vision in an amblyopic eye cannot be improved with glasses, surgery or other interventions. Importantly, a person’s loss of visual acuity (VA) is not the result of any structural abnormality of the eye. Rather, it is due to the “wiring” between the eye and the brain, which, for various reasons, has failed to develop normally during childhood. In this piece, we’ll talk more about why amblyopia develops, how it is detected, and what can be done to treat it.
There are three general circumstances that disrupt visual processing during the critical period and may lead to amblyopia: Deprivation, uncorrected refractive errors, and strabismus.
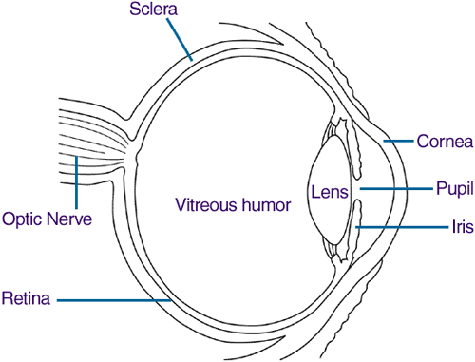
The second subtype, refractive amblyopia, occurs when abnormal vision stems from uncorrected refractive error, most commonly hyperopia (farsightedness) or astigmatism (irregular curvature of the cornea), at a young age. Visual images in both eyes are degraded, resulting in abnormal visual processing. Getting the visual problem corrected can improve visual acuity, but still may not achieve normal sight for one’s age.
Early intervention is essential for correcting visual problems, in order to reduce the likelihood of permanent vision loss.
Anisometropia is the most common cause of refractive amblyopia. This happens when there is a difference in the refractive error (strength of the glasses prescription) between the two eyes, which leads to a difference in quality of the images projected onto the fovea. Specifically, one eye sees a more blurred image than the other eye. If accurate glasses are not prescribed or worn, connections between the eye with the blurred image and the brain fail to form and those from the sound eye expand. Indeed, fMRI studies show that if the defect develops in infancy, the healthy eye occupies more space in the brain’s visual cortex than the amblyopic eye.
The third type of amblyopia, strabismic amblyopia, is fundamentally different. Here, misalignment of the eyes results in a different image being cast onto each eye. Despite this misalignment, children with the condition rarely have double vision because the image from the non-dominant eye is actively suppressed (i.e. ignored) by the brain. Chronic suppression can result in amblyopia.
Amblyopia is a disorder of brain development (in particular, the primary visual area, V1), although again, there are many different specific mechanisms that can lead to the condition.
Researchers have this process pretty well mapped-out in animals. The precise timing of critical periods in human children is less clear, but researchers are learning more. For example, it is known that binocular function can be damaged by deficits that occur up to 24 months of age, while amblyopia can develop up to age eight. We also know that amblyopia is a disorder of brain development (in particular, the primary visual area, V1), although again, there are many different specific mechanisms that can lead to the condition. Early intervention is essential for correcting visual problems, in order to reduce the likelihood of permanent vision loss.
The prevalence of amblyopia is approximately 2.5% in the general population, and boys and girls are affected equally. Occurrence of amblyopia does vary with ethnicity, with a prevalence of 1.5% among African-American children and 2.6% among Hispanic children. The majority (75%) of amblyopia cases are caused by refractive error, mentioned earlier (anisometropic amblyopia being the most common subtype). Strabismus is the next most common cause of amblyopia and deprivation amblyopia is least common, but the most visually devastating.
For the reasons just mentioned, early detection through screening is critical. Screening can be performed through many sources, including schools, pediatricians, eye care professionals and automated photo-screening programs. Each of these routes has its pros and cons, since access, efficacy and cost vary with each approach. While mandatory eye exams have been advocated in some states (Missouri, Illinois and Kentucky), this may not be the best strategy because of they can be expensive and not always easily accessible, limiting compliance with exams. (According to the Missouri Children’s Vision Commission, less than 40% of children required to obtain mandatory eye exams in Missouri prior to kindergarten actually got them during the years 2008-2010.).
Studies have shown that lay testers, armed with the right screening tools, can detect the disorder successfully in children as young as 3.
Federal initiatives to expand vision screening for children will increase the number of children identified with amblyopia. While the benefits of identifying and treating the condition are undeniable for the child, whether the cost to society for the screening and identification of that one child is acceptable is a source of debate. Studies have shown that lay testers, armed with the right screening tools, can detect the disorder successfully in children as young as 3.
With cheaper and more reliable screening tools, the balance falls in favor of screening – both more often and younger. New directions in screening include home-based screenings. In one study, home-based amblyopia screening packages were distributed to parents through the kindergartens, and children were later examined by an eye care professional. The screening package was found to be quite accurate. The total cost for screening out one child with amblyopia was just $266.00.
Occlusion therapy – patching the healthy eye – has long been the mainstay of amblyopia treatment. However, daily time spent patching and duration of treatment had not been established. The Pediatric Eye Disease Investigator Group (PEDIG) initiated the first of several Amblyopia Treatment Studies (ATS) to examine the many questions surrounding the treatment of amblyopia.
Amblyopia is typically classified by type and severity. Moderate amblyopia is defined as best corrected visual acuity (BCVA) between 20/40 – 20/80, while BCVA between 20/100 - >20/400 is classified as severe amblyopia. BCVA better than 20/40 is considered mild.
One issue that has been raised is the recurrence rate of amblyopia once treatment is discontinued.
The first ATS study examined patching versus an eye drop treatment called atropine penalization for moderate amblyopia. Children ages 3-7 with moderate amblyopia were randomly assigned to patching or atropine, which dilates the pupil and blurs the vision (thereby “penalizing”) the “good” eye in order to strengthen the amblyopic eye. Improvement in BCVA was initially faster in the patching group, but equalized after six months. Atropine was found to be both cheaper and easier.
Severe amblyopia can be treated with either full-time or part-time patching of the “good” eye. Full-time patching is defined as patched for all waking hours, part-time patching occurs for six hours per day. After four months of patching the good eye, children treated with either full- or part-time patching had similar, improvement in vision: they could read an average of four lines further down the eye chart. An even greater treatment effect was seen in people who had worse vision to start with.
Another study found that two vs. six hours a day of patching had about the same effect for moderate amblyopia. Finally, yet another study looked at the frequency (weekend-only versus daily) of atropine administration in moderate amblyopia. Weekend-only atropine provided an improvement in visual acuity similar to that seen with daily atropine, but people forget to put in atropine more often if they were not using it daily.
One issue that has been raised is the recurrence rate of amblyopia once treatment is discontinued. One study found that vision worsened in 25% of patients when they finished treatments with either atropine or two-hour patching, while 42% of patients using six hours of patching regressed. It may be that patching should be “weaned” from six to two hours in patients who initially start out with longer patching regimens.
Glasses (“spectacle correction”) may also help children with moderate amblyopia. One study in children aged 3-7 demonstrated that improvement in visual acuity was achieved with eyeglasses alone in both strabismic and anisometropic amblyopia in some children. However, BCVA of 20/25 or better was seen in 74% of children treated with spectacle correction combined with spectacle correction as compared to 43% of children treated with spectacles alone.
Many different factors contribute to the outcome of treatment for amblyopia, including the underlying cause of amblyopia, a child’s initial visual acuity (or the severity of amblyopia), the age of the child, and the type of treatment used.
While all forms of amblyopia can cause reduced vision in the affected eye, their treatments and prognoses differ.
- Deprivation amblyopia requires fast treatment of whatever is compromising the visual input, followed by intensive amblyopia treatment. Otherwise, these eyes have very poor potential for improved vision.
- Refractive amblyopia is usually discovered at older ages (because the child’s eyes are not obviously misaligned and the non-amblyopic eye has normal vision), which limits the time for intervention and correction.
The initial vision in the amblyopic eye may affect the amount of improvement seen with the first treatment. One study grouped patients based on the acuity of vision in the amblyopic eye (20/100 or worse, 20/80 - 20/50, and 20/40 or better), the 20/100 or worse group improved the most. This suggests that even those eyes with severe loss of vision from amblyopia have the greatest potential for improvement with treatment.
The age of the child at the start of amblyopia treatment is also quite significant. Younger children seem to have the greatest benefit from treatment, and children over the age of seven are less responsive than younger children to amblyopia therapy. In eyes with severe amblyopia, children age 3 to 5 were somewhat more responsive to either six hours/day of patching or full-time patching than were even slightly older children (5 to 7).
In eyes with severe amblyopia, children age 3 to 5 were somewhat more responsive to either six hours/day of patching or full-time patching than were even slightly older children (5 to 7).
Yet older children still show improvement with amblyopia therapy. Among children aged 7-12, 17, 25% had improved visual acuity with spectacle correction alone. Fifty percent (50%) of children age seven to 12 saw an improvement in visual acuity with the addition of 2-6 hours of patching with or without atropine. This was true even if the amblyopia had been previously treated. Even among older children aged 13-17, 25% of the group using patches or atropine and 23% of the glasses-only group had an amblyopic eye that showed significant improvement in vision.
Surprisingly, among the older children without a prior history of treatment, twice as many showed significant gains in vision with glasses and two to six hours of patching (50%). This means that amblyopia responds to treatment even after age seven, challenging the earlier belief by many eye care professionals that intervention above a certain age is ineffective. Therefore, these studies have effectively removed the “statute of limitations” on the treatment of amblyopia, confirming that atropine and patching can still improve the vision of older children with unilateral amblyopia.
An area of ongoing interest is whether vision can improve in adult patients with amblyopia. The fact that older children without a prior treatment history show improvement suggests there may be hope after the critical period in early childhood. Patients with strabismic amblyopia may show a “slippage” of visual acuity in the amblyopic eye long after early childhood. This acuity loss can be reversed with patching or penalizing the healthy eye even in adults, although it may subsequently “slip” again after the therapy is stopped.
Recently, a concept called perceptual learning – the act of repeatedly practicing a challenging visual task – appears to bring substantial and lasting improvement in vision. In patients with amblyopia, improvements learned over time have been shown to generalize to other, newer tasks. This may translate to improvements in visual acuity.
Occlusion treatment (eye-patching) for strabismus was first described in 1722. Given the challenges, which include the social stigma of wearing an eye patch and the likelihood that people may discontinue treatment (both with patching and atropine treatment), alternative therapies are attractive.
Opaque contact lenses (CTL) are designed for extended wear and reduce visual stimulation significantly if used in the sound eye instead of patching. The efficacy of opaque CTLs was examined in a group of children who did not tolerate patches and who had failed conventional treatment. In the study, 92% of patients improved at least one line of visual acuity. However, in 11 of 25 patients, their amblyopia returned (although to a reduced level) when the CTL was discontinued. Another study found that opaque CTLs in children over five showed that they can be an effective alternative to patching, although lens hygiene and handling issues may exist. Nonetheless, they remain a treatment option for some patients, particularly since they allow for the avoidance of the social stigma associated with patching.
Another method is known as silicone-eyelid closure. In this method, the good eye is closed using a silicone piece which helps keep the good eye shut. Two to four weeks later, the suture is cut and the silicone sleeve removed. This method had promising results for people with severe amblyopia, and does not affect vision in the healthy eye at all, which is important.
An entirely different treatment for amblyopia is that of pediatric refractive surgery for patients who have not been able to use glasses or contact lens therapy.
Pediatric laser refractive surgery was first reported in 1995. Photorefractive keratectomy (PRK), laser epithelial keratomileusis (LASEK) and laser-assisted in situ keratomileusis (LASIK) have all been used in the pediatric population. Surface ablation techniques include LASEK and PRK. Studies have found good improvement in both visual acuity and stereopsis (i.e., depth perception—which requires visual input from both eyes) with LASEK. One found that visual acuity improved in 97% of the children, and an impressive 69% gained binocular vision. Complications of the procedures can occur but they are typically manageable with topical medications.
LASIK uses a laser to remodel part of the cornea. Results have suggested that pre- and post-operative visual outcomes were similar in LASIK and other procedures.
Implantation of intraocular lenses, either following removal of the lens or as a secondary IOL, is another form of surgery that has had encouraging results. Eighty-five percent of patients had improved functional vision with significantly improved uncorrected visual acuity. and patients often report improved physical coordination and reading and writing skills. There are several types of IOLs available, each associated with different risks for benefits and complications.
Amblyopia is not just a childhood condition: The impact of having decreased vision as a result of amblyopia extends into adulthood. Amblyopia is also a significant public health problem, as it is the leading cause of one-sided vision loss in young and middle-aged Americans. As discussed above, early detection and treatment is still the most effective way to prevent decreased visual acuity or impaired binocular vision.
People with impaired vision, even if the impairment is just on one side, are more likely to have an unskilled manual labor job and to be unable to work because of permanent illnesses. And worsening distance vision also has negative social and economic impact. Amblyopes have poorer fine motor skills compared to others, in addiction to impaired binocular vision. Amblyopia may even be associated with a borderline significant decreased rate of completion of university degree, although that finding has not been reproduced in all studies
While the majority of people with amblyopia have excellent vision in their healthy eye, they are at greater risk of lifetime visual impairment due to loss of vision in the good eye. People with an amblyopic eye have nearly three times the risk of vision problems compared with people who do not have amblyopia. Young adults have an increased risk of a traumatic eye injury in their better seeing eye and older adults have greater rates of macular degeneration.
Screening by eye-care professionals can result in the unnecessary prescription of glasses, potentially increasing the costs associated with amblyopia screening. This is likely because mild farsightedness is normal in young children and does not require correction.
Most state agencies define visual impairment as best-corrected vision of 20/60 or worse in the better-seeing eye, which allows an individual to be eligible for special services and accommodations. Detection and treatment of amblyopia, therefore, can prevent blindness and its additional cost to society. This benchmark is fairly low: identifying and treating just 12.5 individuals with amblyopia allows for the successful prevention of one case of visual impairment in both eyes.
The increased risk of bilateral visual impairment among people with amblyopia underscores the need to screen for and treat amblyopia. Screening is vital to preventing visual loss from amblyopia, especially for people with the anisometropic subtype, who often do not have symptoms early in the course of the disease. While no randomized studies have demonstrated that screening directly reduces rates of blindness, we know that as people age, the visual system does not respond as well to delayed treatment of amblyogenic factors and that, therefore, the most successful programs would screen the very young and refer affected individuals to an eye care professional for diagnosis and management.
For this reason, the American Association of Pediatrics recommends eye screening as a component of the yearly well-child visits starting at age 3 in addition to school-based screening programs. Additional focus on screenings by laypersons with referral back to the pediatrician for children who fail will increase the chance of identifying children with visual problems at earlier ages.
Another approach advocated by some includes mandatory comprehensive eye exams. However, professional eye examinations may not be the best approach. In fact, in states where such exams have been mandated, these programs have sizable direct and indirect costs and yet still fail to screen the majority of children.
Furthermore, one study suggests that screening by eye-care professionals can result in the unnecessary prescription of glasses, potentially increasing the costs associated with amblyopia screening.40 This is likely because mild farsightedness is normal in young children and does not require correction. In a study of glasses prescribing patterns, both optometrists and comprehensive ophthalmologists (eye MDs not specializing in treating children) prescribe glasses to over half of children with insignificant hyperopic refractive error (farsightedness). The glasses given in these circumstances are quite weak despite studies that show no benefit to prescribing glasses for these low levels of hyperopia.41. In fact, in this study glasses were never prescribed to a child having mild farsightedness by an “experienced” pediatric ophthalmologist (eye MDs who have specialty training in pediatric eye disease). The author concludes that if all US children were required to have screening eye exams by eye care professionals not be familiar with appropriate spectacle prescribing practices (or possessing ulterior motives for recommending glasses such as aclinic-owned optical shop, for example), it is estimated that over $200 million would be spent on unnecessary glasses yearly.
During the last decade, detection and treatment of amblyopia have received increased attention as we recognize the psychological and social impact of amblyopia and the economic effects of sight in only one eye. Ideally, making screening as inexpensive as possible – through the use of photoscreeners and layperson evaluations, will improve both the access to and the identification of young children affected by amblyopia. This strategy would have the added benefit that by improvingthe cost-effectiveness of screening for the general population may tip the scales to the point where the cost screening is offset by the cost savings to society in the form of reducing the burden of visual disability.
The goal of this article is to assist the general public, teachers, patients, and especially their parents in understanding the significant risk of visual disability from amblyopia. There are typically few symptoms associated with amblyopia, complicating its detection and potentially delaying its treatment. The strategy for amblyopia detection is to screen early and screen often: at well-child visits, in daycare centers, at health fairs, and in the schools. There are many treatment options for children identified with amblyopia, ranging from glasses, penalization of the “good” eye, eye muscle surgery, and refractive surgery. Hopefully, the visual complications of amblyopia and the availability of treatment should motivate eye care providers to work together with school nurses, pediatricians, and parents to identify those children at risk for amblyopia and refer to an eye-care provider for a comprehensive evaluation.




