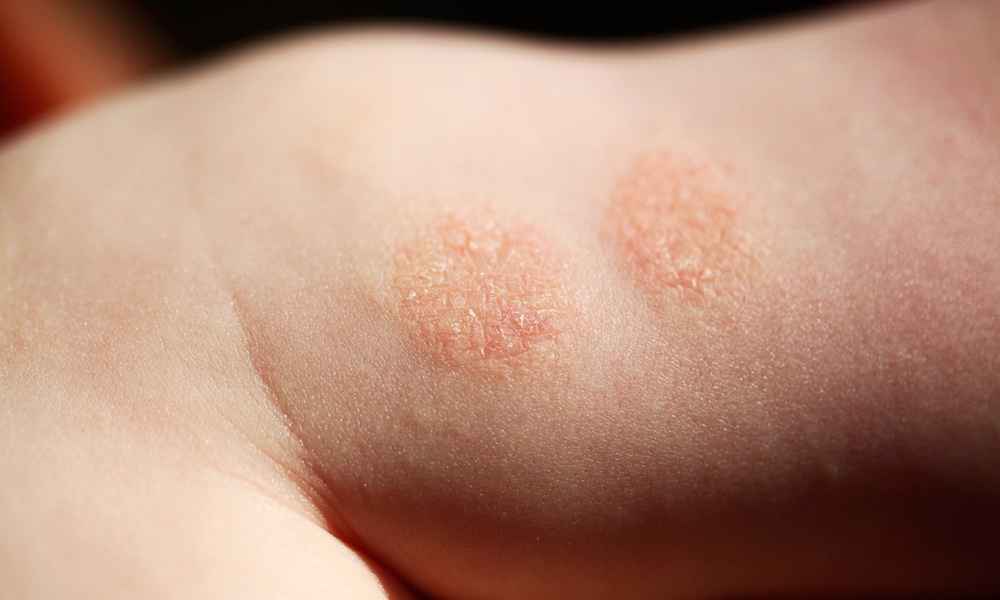
When children have red itchy patches on their skin the diagnosis is usually atopic dermatitis, a common type of eczema, that most often develops by the time a child is five-years-old. Other symptoms include:
- Dry scaly skin
- Severe itching
- Redness and swelling
- Thickened skin
- Pale skin on the face
- Small, raised bumps that may become crusty and leak fluid if scratched
- Rough bumps on the face, upper arms, and thighs
- Darkened skin on eyelids or around the eyes
But these symptoms may not be enough for a complete diagnosis. It can be a good idea to offer young patients a test to see if they have contact dermatitis, another eczematic skin ailment in addition to atopic dermatitis, a recent study suggests. Contact dermatitis is an allergic reaction that is usually triggered by exposure to irritating, allergenic substances like cleaning supplies and other environmental chemicals.
Contact dermatitis most often shows up in the form of a rash, hives or red, itchy bumps and it is caused by contact with something to which the child is sensitive or allergic, such as poison ivy, jewelry (often from nickel exposure), sunscreen and other lotions, rubber, even some hand sanitizers.The treatment for contact dermatitis is different from that for atopic dermatitis. The most effective way to treat allergic contact dermatitis is by identifying and then avoiding those substances that cause the allergic reaction.
“When a dermatologist sees a child who looks like they have eczema, we usually think that it's atopic dermatitis because nearly 1 in 5 children develops it,” said the senior author of the study, board-certified dermatologist JiaDe (Jeff) Yu, assistant professor of adult and pediatric dermatology at Massachusetts General Hospital.
“Sometimes these kids could have allergic contact dermatitis, but the only way to tell is through patch testing, which is designed to identify substances that may be irritating your skin,” he said in a journal news release.
During patch testing, different substances are placed on the skin and taped in place. The patches are typically put on the back, left on for 2 days and then removed. The area of skin that was tested will be evaluated by the dermatologist 2 to 4 days after the patches are removed. Keeping a record of activities and possible items that may have triggered an allergic reaction can also better enable a doctor to identify the allergen or irritant. A list of what has touched the child's skin over a 48-hour period can help to reduce the number of possible culprits.
While the treatment for atopic dermatitis includes steroids applied to the skin and phototherapy, which uses ultraviolet light to reduce inflammation and ease itch, as well as medications called biologics and JAK inhibitors (used to treat inflammatory disorders), the treatment for contact dermatitis is different. The most effective way to treat allergic contact dermatitis is by first identifying and then avoiding those substances that cause the allergic reaction.
Lifestyle changes can also relieve the symptoms of contact dermatitis. Choosing fragrance-free products, for example, can help limit eczema flares. Also, kids with eczema should not use new skincare products (including sunscreen) without first applying them to a quarter-sized patch of skin on the inside of the arm every day for four weeks before using the product more widely.
“I imagine it like layers of a cake,” Yu said. “Maybe the first layer is atopic dermatitis and the second layer is allergic contact dermatitis. In these cases, the overall eczema may look very severe, but once you remove the allergic component, the eczema seems much more manageable.”
If your child is showing signs of any type of eczema it is important to see a board-certified dermatologist to get a diagnosis and an effective treatment plan. You can find a dermatologist in your area at: www.aad.org/findaderm
The article can be found in the Journal of the American Academy of Dermatology.