Dr. Alnigenis is a Visiting Fellow in the Division of Rheumatology, Montefiore Medical Center, Bronx, N.Y.
Fibromyalgia Syndrome (FMS), is an illness that causes pain, stiffness and tenderness throughout the body. Sufferers complain they have trouble sleeping and tire easily. 80%-90% of FMS victims are women and most are between 30 and 60 years old.
Though FMS may not be well understood, it is far from uncommon. A recent study found that 2% of all North Americans suffer from FMS, 3.4% of women and 0.5% of men. It is the second most common problem seen by rheumatologists in North America.
Some doctors believe that FMS is not a real condition, but, instead, is psychological. What do we actually know about FMS?
How FMS Starts
A possible clue to the origins of FMS is the fact that sufferers often report that their symptoms began after they came down with another illness or went through some other kind of health problem or personal crisis. The most common of these events are listed in Table 1.
Table 1.
Events Linked to the Onset of FMS9
- Flu
- HIV infection
- Parvovirus
- Lyme disease
- Toxic oil syndrome
- Siliconosis
- Problems sleeping
- Physical trauma (e.g., whiplash injury)
- Emotional trauma
- Withdrawal from steroids or other medication
- Stressful event
Pain and Fatigue
The main symptom of FMS is chronic widespread pain. Generally, the patient "hurts all over," but has difficulty pinpointing the location. The pain typically comes and goes, varying in intensity. Flare-ups often follow unaccustomed exertion, physical injury, a period of sleeplessness, exposure to cold or a stressful event.
Another common symptom is profound fatigue. This often peaks after getting out of bed in the morning or in the mid-afternoon. Even minor activities can aggravate the pain and fatigue but so can prolonged inactivity. Patients awake in the morning feeling stiff and unrefreshed, even if they have slept 8 or 10 hours. Many patients do not complain of severe sleep disturbances, but do sleep lightly and wake up frequently during the night. The most common FMS symptoms and factors that seem to exacerbate or alleviate these symptoms are listed in Table 2.
Table 2.
FMS Symptoms and Aggravating Factors
| Symptoms | Factors that make FMS symptoms better or worse |
|---|---|
|
|
FMS cannot be detected in a normal physical exam. Nor does it show up in a neurological exam, x-ray or standard laboratory tests. The symptom that most often leads to the discovery of FMS is the existence of what are called tender point sites. Tender point sites are specific areas of muscle, tendon or other tissue that are painful to the touch. FMS patients are not often aware of the exact location of many of these points. Figure 1 shows the 18 tender point sites that have been identified by the American College of Rheumatology (ACR). According to the ACR criteria, FMS is present when a patient suffers widespread pain for at least three months and feels pain in 11 or more of the 18 pressure point sites.
Figure 1.
Eighteen tender point sites of FMS
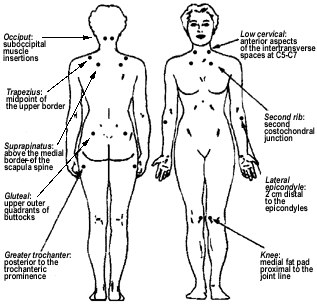
Doctors measure these tender points in one of two ways: by simply pressing the site with a finger or by using a slightly higher-tech method called dolorimetry. In the dolorimetry method, the examiner presses a rubber endplate, attached to a spring-loaded force gauge, into the tender point site with increasing force. Patients are then asked to say when they stop feeling pressure and start feeling pain.
FMS and Other Disorders
Patients with FMS often suffer from associated diseases. The most common of these are listed in Table 3.
Table 3.
Illnesses that Often Accompany FMS
- Rheumatoid Arthritis (12% of FMS sufferers)
- Systemic Lupus Erythematosus (22% of FMS sufferers)
- Primary Sjogren's Syndrome (11% of FMS sufferers)
Table 4.
Diseases that Mimic FMS
- Polymyalgia rheumatica
- Myositis or myopathies
- Neuropathies, multiple sclerosis, or myasthenia gravis
- Spondylarthropathies
- Hypermobility disorders
- Substance abuse
- Endocrinopathies: hypo/hyperthyroidism, diabetes, hypoglycemia, and parathyroid disorders
Also complicating the FMS picture is the fact that FMS sufferers often have a variety of overlapping conditions or syndromes. The most common of these are shown in Table 5.
Table 5.
Conditions that Often Overlap with FMS
- Depression
- Restless leg syndrome
- Irritable bowel syndrome
- Irritable bladder syndrome
- Migraine
- Chronic fatigue syndrome
- Myofascial pain
- Multiple Chemical Sensitivity Syndrome
Is FMS Really Psychosomatic?
As with other diseases whose causes are not understood, some have suggested that FMS may be a psychosomatic illness or even a psychiatric disorder. In the past, FMS patients have been diagnosed as hysterical. It is not hard to understand why: FMS sufferers look well and have normal laboratory test results. Their chief symptom, pain, is quite subjective and is difficult to document. In addition, many FMS symptoms also occur in depression and other psychiatric problems. Chronic pain, for example, can accompany anxiety and depression; clinical depression can cause fatigue, sleep disturbance and pain. Some researchers go so far as to question whether FMS even exists as a physical illness. In one study of childhood experiences, FMS patients were found to be much more likely than others to have experienced maltreatment or victimization.
Though psychiatric problems do not cause tender point sites (the chief distinguishing feature of FMS) and we know that FMS patients who have been cured of depression normally continue to suffer from FMS, there does seem to be a relationship of some kind between FMS and various psychiatric disorders.
Furthermore, studies have found that FMS sufferers, when compared to rheumatoid arthritis patients, are much more likely to have a psychiatric diagnosis at some point in their lives, and are much more likely to experience medically unexplained physical problems.
Possible Causes of FMS
While we do not know with certainty the causes of FMS, there are several theories. These include muscle abnormalities that might account for tender point sites; central nervous system abnormalities that might cause sleep disturbance and sensory problems; and problems with neurohormones (serotonin, endorphins, growth hormone) or other bodily substance that might lead to amplified pain perception.
How to Treat and Manage FMS
Recommended treatments include:
- Dealing with any overlapping disorders.
- Controlling aggravating factors (e.g., barometer changes, humidity, cold, warmth, noise).
- Modifying lifestyle: (e.g., healthy diet, changes in working conditions, preventive medicine).
- Managing pain using non-narcotic analgesics (acetaminophen, tramadol) and heat and cold treatments. Narcotic analgesics should be used sparingly and only under unusual circumstances.
- Improving sleep quality by analysis of sleep, treating sleep disturbances (e.g., sleep apniea, restless leg syndrome), improving sleep hygiene, and with medications (zolpidem tartrate).
- Dealing with fatigue: optimizing rest and activity, pacing yourself.
- Using EMG-biofeedback, acupuncture or hypnosis therapy.
- Embarking on a low-impact exercise program (i.e., brisk walking, biking, swimming or water aerobics), plus strengthening and stretching exercises.
- Dealing with stress, depression, and problems such as alcoholism and childhood abuse with cognitive behavioral therapy, counseling, relaxation techniques and self-help groups.
- Patient education. The patient must understand that this disorder is neither life threatening nor imaginary. Educational literature from the Arthritis or Fibromyalgia Societies and access to support groups can reduce patient anxiety and play an important role in FMS treatment management. See the list of FMS internet sites below:
- Fibromyalgia i>Network
- Oregon Fibromyalgia Foundation
- National Fibromyalgia Research Association
Besides the painkillers and drugs already mentioned, there is a wide variety of other drugs that can be effective in treating FMS. These are almost always given in combination with one or more of the non-drug therapies listed above. They include:
Nonsteroidal anti-inflammatory drugs (NSAIDs)
Tricyclic antidepressants (TCAD): TCADs can decrease depression, relax muscles, improve sleep, and release endorphins. Side effects include weight gain, constipation, low blood pressure, agitation and morning hangover.
Serotonin reuptake inhibitors: morning administration of these drugs may relieve daytime fatigue and fight pain.
Muscle relaxants
Benzodiazepins: these promote sleep, relax the muscles and help restless leg syndrome.
Local injections with lidocaine and steroids.
Topical creams: capsaicin 0.25%.
Summary
FMS is a difficult and poorly understood illness that affects different people in different ways. Accordingly, there are many approaches to its treatment and therapies must be customized to the needs of the individual FMS sufferer.




