- acute, which is often related to an associated disease
- chronic persistent incontinence.
Acute Incontinence
Acute incontinence appears suddenly and is not rare in older individuals. It is usually associated with an underlying disease. The causes of acute incontinence are best remembered by the mnemonic, DRIP:
- Drugs, delirium
- Retention of urine, Restricted mobility
- Impaction, Infection
- Polyuria, Prostatism
The treatment of acute incontinence includes frequent toileting and treatment of the underlying cause. Catheterization should be avoided as it increases the likelihood of hospital-acquired infections.
Chronic Incontinence
The types of chronic incontinence are:
- Urge incontinence, the most common form of incontinence, is characterized by loss of small or large volumes of urine when the individual has insufficient warning, following the first urge to void, to allow him or her to reach the toilet.
- Stress incontinence occurs in women who usually have had children and is characterized by loss of small volumes of urine following coughing, sneezing or other maneuvers that increase intra-abdominal pressure. It happens because the internal urethral sphincter, the circular band of muscle that surrounds the bladder opening, has lost muscle tone and pushed outside of the abdominal cavity.
- Reflex incontinence occurs in persons with spinal cord damage. Their bladders do not receive, via the spinal cord, the message to stop urination.
- Functional incontinence occurs when either a person's physical or mental state deters the person from urinating in the toilet, i.e., the person lacks the physical ability to reach the toilet or lacks an adequate thought process to go to the toilet when having the urge to urinate. Causes include strokes, dementia and depression.
- Overflow incontinence is of two types:
- Neurogenic - the individual does not receive a message that the bladder is full and a signal to urinate is not transmitted. This occurs in persons with autonomic neuropathy.
- Obstructive - prostate enlargement is the usual cause.
Diagnosis
A careful history by the doctor and bedside investigation of urine flow (urodynamics) are necessary:
The patient empties their bladder and then, lying on the examination table with a bedpan underneath them, is asked to cough. Loss of urine indicates stress incontinence. The patient is then catheterized and urine drained. If there is more than 100 cc, the person has overflow incontinence. A 50 cc syringe is then attached to the catheter and the bladder is filled with normal saline. The patient is asked to indicate when the first urge to urinate is felt. If this occurs before 300 cc or if it is accompanied by immediate, vigorous movement of the bubble in the syringe, the diagnosis is urge incontinence. When 400 cc of saline has been instituted into the bladder, the catheter is removed and the person is asked to cough again. Loss of urine = stress incontinence. The patient is then asked to void into a container. If greater than 100 cc, then overflow incontinence is diagnosed.
Management of Incontinence
Table 1 below provides a useful summary of the treatments for various types of incontinence.
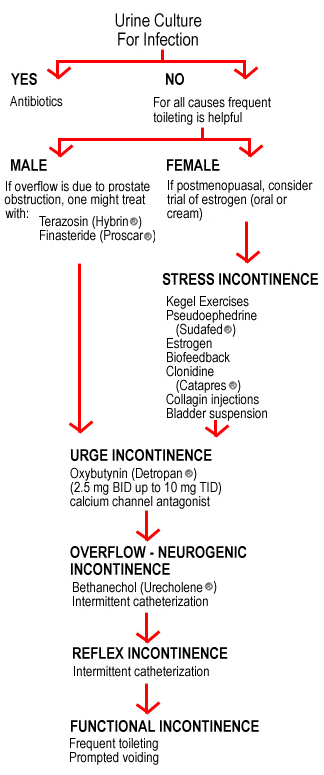
Finally, remember that many older persons develop DHIC (detrusor hypercontractibility and impaired contraction), a combination of urge and neurogenic incontinence. Treatment depends on needs of patient, e.g., if being wet during the day is unacceptable, then oxybutynin is given in the morning and bethanechol in the evening.
Conclusion
Urinary incontinence is a straightforward condition, its cause easily identified and treated. Treatment can have a major impact on the older person's quality of life. Proactive preventive Kegel exercises may be helpful.




