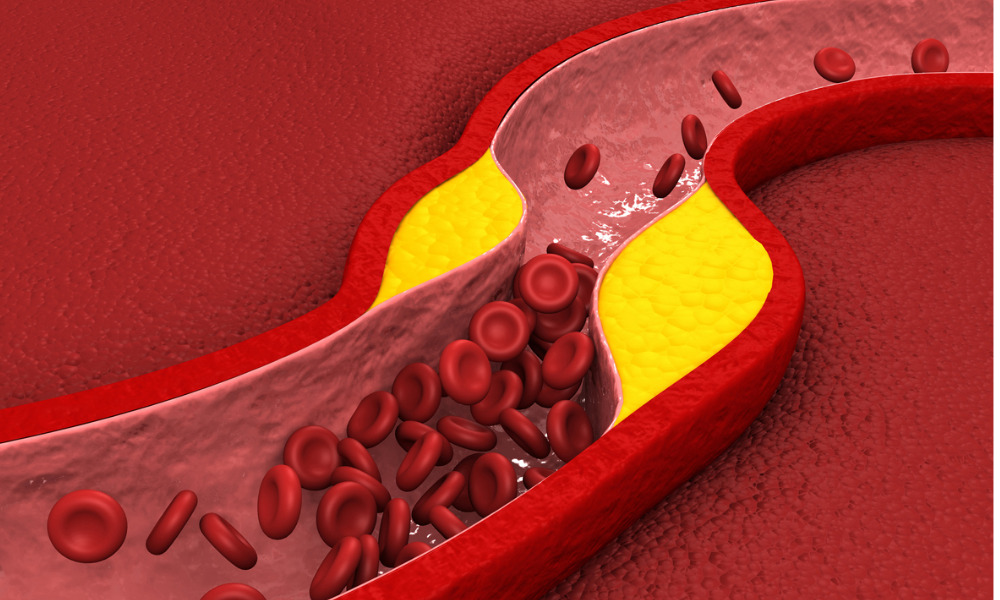
In the 1970s, the Framingham Heart Study made the connection that high-density lipoprotein cholesterol (HDL-C) levels reduced a person’s risk of cardiovascular disease (CVD) and heart attacks, as well as deaths from heart attacks.
The finding led to HDL-C, or HDL as it more commonly known, being dubbed the good cholesterol. Low-density lipoprotein cholesterol or LDL, which increased the risk of CVD events, became known as the bad cholesterol.
Later studies that confirmed these associations were done primarily in white, European populations. The protective effect of HDL was weaker or absent in more racially diverse study populations, but these studies did not specifically look into the link between race and the protective effects of HDL.
A new study by American researchers has found that HDL levels may not be as strong a predictor of CVD risk as previously believed among adults of different racial and ethnic backgrounds. Low levels of HDL increased the risk of CVD events in white participants only. And high HDL levels did not decrease the risk of CVD events in participants of either race.The fact that low HDL levels only increased the risk of cardiovascular events in white participants was the most surprising finding.
Data from almost 24,000 participants in the REGARDS (REasons for Racial and Geographic Differences in Stroke) cohort were analyzed for the current study. Participants were 45 years of age or older and had never been diagnosed with CVD. During the 10- to 11-year follow-up period, 664 Black participants had heart attacks or heart attack-related deaths. About 950 white participants had CVD events.
“I hope this type of research establishes the need to revisit the risk-predicting algorithm for cardiovascular disease,” Nathalie Pamir, a senior author on the study, told TheDoctor. It could mean that physicians won’t be congratulating patients on raising their HDL levels in the future, she added.
Pamir, an associate professor of medicine at Oregon Health and Science University, said the fact that low HDL levels only increased the risk of CVD events in white participants was the most surprising finding. “We had previously accepted that low levels of HDL-C are bad for everyone. We showed it is only bad for white Americans,” she said.
Measures other than HDL levels may play a role. The authors point to several possibilities that may explain the race-specific association of HDL with CVD risk: the number of small versus large HDL particles; the amount and type of proteins in HDL; and antioxidant, anti-inflammatory and cholesterol removal activity.
In addition, race is a complex trait, and more studies are needed to understand how racial differences operate. “There is much more to race than ethnicity. We are trying to better understand what is coming together under the race umbrella that will modify disease risk,” Pamir said.
The study and a related editorial are published in the Journal of the American College of Cardiology.