Dr. Ramsay is a Fellow, Division of Geriatric Medicine, St. Louis University School of Medicine. He reports no commercial conflict of interest.
Exercise can be defined as sustained physical activity which is planned, structured and involves repetitive movement aimed at improving or maintaining one or more components of physical fitness.
Data drawn from the National Health Interview Survey, Federal Centers for Disease Control (CDC), and National Health Center for Health Statistics in 1995, indicated that approximately 16 percent of Americans engaged in regular vigorous physical activity three days per week. Twenty-five percent were completely sedentary. In 1997 data reported to the National Health Interview Survey showed a decrease in physical inactivity with aging.
Table 1.
Physical Activity By Age Group.
| Age group |
% No physical activity |
% Vigorous physical |
| 18 to 24 years |
31 |
32 |
| 25 to 44 years |
34 |
27 |
| 45 to 64 years |
42 |
21 |
| 65 to 74 years |
51 |
13 |
| 75 years and older |
65 |
6 |
Adapted from The National Health Interview Survey 1997.
The Surgeon General's report on physical activity and health in July 1996 concluded that regular sustained physical activity could substantially decrease the risk of developing heart disease or dying from it. The report hoped to motivate Americans to engage in regular physical activity. Prescribing exercise should be regular practice for all clinicians and the following includes guidelines for doing so.
Exercise can be divided into four main categories:
- Resistance training
- Aerobic training
- Balance training
- Flexibility training
Resistance Training
Resistance or strength training builds muscle strength and mass. Nelson et al. showed that age-related loss of strength, muscle mass and bone density, especially in women, could be lessened by strengthening exercise begun in middle or old age. Gains in muscle strength in frail elders may enhance balance, aerobic capacity, flexibility, and performance-based tests of functional limitation, such as gait velocity, stair climbing and the get up and go test. Most low to moderate intensity resistance training programs, however, do not substantially improve strength.
Psychological responses were also seen with resistance training. These included improved morale and reduced depressive symptoms. In two studies, high intensity progressive resistance training and aerobic training, reduced depression to a similar extent as medications.
Resistance training involves use of weights in isometric and isokinetic training. Most programs for elders utilize free weights, elastic bands or body weight to provide resistance. Training protocols are based on weight and number of repetitions. The weight used is determined by the maximum weight the person can lift just once (1-RM or one repetition maximum). Common protocols use 2 to 3 sets of 8 to 10 repetitions each. Resistance training itself has different subgroups.
Progressive resistance training may start at 75% of the 1-RM with an increase in resistance with each set. Fixed resistance training uses the same weight for all sets. Progressive rate training uses the same weight but increases the rate with each set.
Aerobic Training
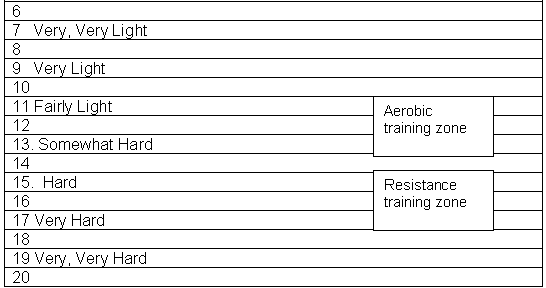
Aerobic training, or endurance exercise, improves aerobic capacity. It involves activity aimed at raising the heart rate to a target of about 60% to 90% of maximum predicted heart rate. In the elderly, your program or trainer need to be aware of age-related physiological changes and use the Borg Scale of Perceived Exertion,(20) to set the maximum activity level. The scale grades perception of exertion (see Table 2). Aim for 11-17 on the scale depending on the mode of exercise.
Table 2.
The Borg Scale of Perceived Exertion.
VO2 max (maximum oxygen consumption at maximum exercise) is a measure of aerobic capacity and has been shown to decline with aging. Low to moderate intensity aerobic activity like walking, standing or stationary cycling at 60% of maximum predicted heart rate has been associated with modest improvements in cardiovascularefficiency and mobility tasks. In one study, there was no decline in VO2 max in master athletes who maintained competitive training over a 10-year period. Another showed a decline at each decade that was inversely proportionate to the intensity of exercise. In other words, the less you exercise, the more your aerobic capacity will decline.
Balance Training
Exercise programs that include balance training have been shown to improve performance in clinical tests of elders with mobility problems and functional impairment. Tai Chi has been shown to reduce falls in healthy elders. Other balance training exercises include tandem walking, standing yoga, stepping over objects and standing on one leg.
Flexibility Training
Poor flexibility is associated with aging and disability. There is no evidence that flexibility programs alone, or physical therapy programs focused on range of motion and stretching alone, have any significant impact on disability. Improvement, however, is seen in active range of motion in frail elders who undergo high intensity progressive resistance training.
What are the Benefits of Exercise in the Elderly?
Some of the benefits are listed in Table 3 below. Master athletes maintain high endurance exercise into old age, and the benefit is seen in maintenance of the VO2 max, which normally declines with aging. Aging is also associated with decline in lean body mass, or fat free mass (FFM), and increase in central adiposity which is a risk factor for the metabolic syndrome.
Endurance training raises the resting metabolic rate by about 10% in the elderly, and decreases body fat with most impact on abdominal fat. It does not increase FFM significantly. Resistance training has a similar effect on adiposity as endurance training.
Table 3.
Some Benefits of Exercise.
- Minimize physiological changes associated with aging
- Increase longevity
- Improvement of aerobic capacity, muscle strength and flexibility
- Improvement in physical performance and function
- Improvement in psychomotor skill
- Prevention of falls
- Reduced risk of many chronic diseases
- Improvement of mood and well-being
- Improvement of sleep quality
- Reduced anxiety and depression
Overloading muscle is the only action proven beneficial in preventing loss of muscle mass and strength. The lack of increase in lean body mass is believed to be a result of decline in levels of anabolic hormones like sex steroids, growth hormone and insulin-like growth factor-1. Table 4 shows some physiological parameters can be modified by exercise.
Table 4.
Physiological Parameters of Exercise.
| Physiological Parameter |
Aging Effect |
Exercise Effect |
| Maximum aerobic capacity |
Decrease |
Increase |
| Maximum heat rate |
Decrease |
No change |
| Muscle strength |
Decrease |
Increase |
| Neural reaction time |
Decrease |
Increase |
| Oxidative and glycolytic enzyme capacity & mitochondrial volume |
Decrease |
Increase |
| Gait speed |
Decrease |
Increase |
| Maximum cardiac output |
Decrease |
Increase |
| Total energy expenditure |
Decrease |
Increase |
| Total body water |
Decrease |
Increase |
| Protein synthesis rate, protein turnover |
Decrease |
Increase |
| Vital capacity |
Decrease |
No change |
| Lipoprotein lipase activity |
Decrease |
Increase |
| Total cholesterol, LDL cholesterol |
Increase |
Decrease or no change |
| Hormonal & sympathetic system response to stress |
Increase |
Decrease |
| Growth hormone & IGF-1 |
Decrease |
Increase or no change |
| REM and slow wave sleep |
Decrease |
Increase |
| Cognitive processing speed & accuracy |
Decrease |
No change or increase |
| Attention span |
Decrease |
Increase |
There is an inverse linear dose response relationship between exercise and all cause mortality rates in elderly and middle-aged individuals. In other words, the more exercise you do, the better chance you'll live longer. Energy expenditure of 1000 kcal per week reduces mortality by about 30%; and 2000 kcal per week reduces it by about 50%. Middle-aged individuals who changed from sedentary to a more active lifestyle also showed reductions in mortality.
Disease prevention is crucial to maintenance of health in elderly individuals. The evidence supporting exercise in prevention of chronic disease is epidemiological in nature. The preventable diseases are: cardiovascular disease, type 2 diabetes mellitus, osteoporosis, stroke, breast cancer, colon cancer and disability itself. In the Nurses Health Study, habitual exercise reduced disease risk by 40% to 50% at the highest levels compared to sedentary women. Increase in physical activity level in mid- to late-life was also protective against ischemic stroke.
In the Finnish diabetes prevention study, the effect of exercise on glucose intolerance was studied in individuals with a mean age of 55 years. There was a 58% to 80% reduction in incidence of type 2 diabetes over three years in those that exercised compared to the sedentary controls. Campbell and associates reported a decrease fall rate of 30% to 40% over a 2-year period among exercising elderly women over age 80 years. Exercise is complementary to traditional medicine in the treatment of disuse syndromes accompanying chronic disease. Exercise can affect the disease process directly or in-directly. Those diseases on which exercise has a direct impact are shown in Table 5. The beneficial effect is indirect in Parkinson's disease, COPD (emphysema), intermittent claudication (when the legs do not receive sufficient arterial oxygen-saturated blood), and chronic renal failure.
Table 5.
Exercise Benefits in Disease.
| Disease or syndrome |
Suggested mechanism of exercise effect |
| Arthritis |
- Maintenance of cartilage integrity
- Decreased body weight
- Maintenance of muscle & tendon strength
|
| CHF |
|
| Depression |
- Increased self-efficacy
- Decreased depression
- Decreased anxiety, improved sleep
- Improved self esteem
- Decreased body fat and improved body image
|
| Frailty, disability |
- Increased muscle mass & strength
- Increased nutrition intake
- Improved protein utilization from the diet
|
| Mobility impairment & Falls |
- Increased strength & muscle mass
- Improved balance & gait stability
- Decreased fear of falling & depression
- Decreased fat mass & body weight
|
| Stroke |
- Decreased BP, cholesterol and obesity
|
| Osteoporosis |
- Increased bone density & tensile strength
- Increased muscle mass
- Improved nutritional intake
|
| Type 2 diabetes |
- Improved insulin sensitivity, and dyslipidemia
- Improved glucose tolerance occurs before decrease in abdominal obesity
- Increased muscle mass
- Increased GLUT-4 protein
- Reduced visceral fat mass
- Decreased cortisol response to stress
- Decreased BP
|
Urinary stress
Incontinence |
- Improved pelvic floor muscle strength
|
Compared to their sedentary peers, physically active adults are more likely to survive to age 80 years and beyond and to do so with half the risk of dying with disability.46 There are shared demographic characteristics between individuals who exhibit sedentary behavior and those at risk for disability. They are advanced age, female gender, non-Caucasian ethnicity, lower educational level and income.
Risks of Exercise
The risks of performing exercise are small provided all medical conditions are considered. The American College of Sports Medicine (ACSM) suggests screening for the possibility of cardiovascular complications using a simple questionnaire such as the Physical Activity Readiness questionnaire (PAR-Q) by Thomas et al. which was revised in 1999.
Possible complications include:
- Cardiovascular complications
- Injury from falls or poor exercise technique
- Heat stress, more likely in hot environments
- Dehydration from inadequate fluid intake
- Fractures related to osteoporosis
- Bronchoconstriction
- Rhabdomyolysis
The following can minimize complications:
- All exercise programs should be preceded by a warm-up period and followed by a cool down period
- Regular fluid intake is important to maintain hydration
- The environment should be well ventilated and have good lighting
- The temperature should be comfortable
- Participants must wear comfortable clothing and shoes.
The absolute contraindications to exercise are:
- Severe coronary artery disease, unstable angina or recent heart attack
- Decompensated congestive heart failure
- Uncontrolled ventricular arrhythmias (irregular heart beat)
- Uncontrolled atrial arrhythmias compromising cardiac function
- Severe valvular heart disease
- Uncontrolled hypertension >200/105
- Pulmonary hypertension
- Recent pulmonary embolism and deep vein thrombosis
- Acute myocarditis (infection of the heart)
The Exercise Prescription
The benefits of exercise outweigh the risks significantly, and the risks will be further reduced if exercise is prescribed on an individual basis. A useful guide is the health fitness gradient from the World HealthOrganization. It categorizes the elderly into three groups based on fitness, health, and independence:
Group 1: Physically fit, healthy and independent
Group 2: Physically unfit and unhealthy but independent
Group 3: Physically unfit unhealthy and dependent.
These individuals regularly engage in appropriate physical activity. They are physically fit and can perform all activities of daily living (ADLs) independently. In this group, the focus of any program should be to prevent disease and disability. Exercise of moderate intensity is recommended and should be done for thirty minutes, three to seven days per week. These are the ACSM recommendations. The Borg scale should be used to gauge exercise intensity.
These individuals live independently, can perform all their ADLs but do not engage in physical activity. There is musculoskeletal frailty and/or chronic disease in this group, and exercise is necessary to prevent disability. Supervised resistance training seems most effective in this group but it should be supplemented with light or moderate endurance activity to improve cardiovascular fitness.
These individuals are no longer able to function independently in society because of a variety of physical and psychological reasons. They are frail, have high levels of disability, disease and co-morbidity, and are often dependent on others to assist in their ADLs. They live in residential facilities or nursing homes. The aim of exercise in this group is to restore independence in ADLs. To achieve this goal, supervised resistance, balance and flexibility training are recommended. In a recently reported study in frail elderly, intensive exercise training produced greater improvements in the modified physical performance test (PPT) and functional status questionnaire (FSQ) scores, and VO2 max, than low intensity home exercise programs.
Exercise regimens can be designed based on Table 6 below, which considers type of exercise, safety and efficacy. Always begin with warm-up exercises to minimize the risk of injury. For a more detailed discussion of the exercise prescription see review article by Fiatarone Singh (2002).
Table 6.
Exercise Regimens.
Type of
training |
Resistance |
Aerobic |
Balance |
Flexibility |
| How often? |
2-3 days/wk |
3-7 days/wk |
1-7 days/wk |
1-7 days/wk |
| How much? |
1-3 sets, 8-12 reps. Target 8-10 major muscle groups per session |
20-60 minutes each session |
1-2 sets of 4-10 different exercises with dynamic postures |
Major muscle groups. One sustained stretch for 20 seconds. |
| How hard? |
15- 17 on the Borg scale. Use 70-80% of 1-RM. 10 seconds per rep. One minute rest between sets. |
12-13 on the Borg scale or 40-60% of max heart rate. |
Progressively more difficult as tolerated. |
Progress using the neuromuscular facilitation techinique. |
| Safety & efficiency considerations |
- Slow speed, no sudden movements. One day rest between sessions.
- Good form, no compensation from other muscle groups.
- No breath-holding or valsalva during exercise. Increase weight progressively to maintain difficulty. Include power training (may use special equipment).
|
- Low impact exercise. Weight bearing activity preferred.
- Include standing and walking as much as possible.
|
- Safe environment. Dynmaic rather than static modes.
- Graded increase in difficulty and complexity as tolerated.
|
Static stretching. No sudden stretching movements. |
Abbreviations: Reps = repetitions, 1-RM= maximum weight that can be lifted just once.
Adapted from Fiatarone Singh 2002.
Summary
Exercise has many benefits for the elderly but not enough people exercise often enough. Medical professionals and their patients need to work together to encourage more frequent exercise. Bear in mind that there may be cultural barriers to overcome, hence the need for individual attention. Each exercise type benefits different aspects of fitness and so all kinds of exercise should be used.