Author's Note: I would like to thank Dr. Catherine Hammett-Stabler, Associate Professor, Department of Pathology and Laboratory Medicine, University of North Carolina-Chapel Hill, and Associate Director of Core Laboratory (Director: Clinical Toxicology, Clinical Pharmacology, Endocrinology, Pediatric Metabolism, Special Chemistry) McLendon Laboratories, UNC Hospitals, Chapel Hill, NC, for her helpful information and advice for this article.
The two most devastating effects of osteoporosis (OP), hip fracture and vertebral fracture, are the result of people living longer and the altered lifestyle of our modern age. In the United States, poor nutrition, or wrong nutrition, and inadequate activity make the genetic predisposition that many have for fragile bones much worse. Though extra weight some carry strengthens bones, obesity is a false cure for it will also lead to arthritis and obesity related illnesses.
Some Definitions
Primary osteoporosis is age-related bone loss, resulting in fragile bones at increased risk for fracture. Secondary osteoporosis is bone loss caused by medication, cancer, hormone, kidney or other systemic diseases. Although we now identify osteoporosis with a lab result measuring bone density, it is probably more useful to think of the disease as a sign of bone fragility, as an imbalance between bone formation and normal bone loss (resorption) during the lifetimes of men and women. Bone is an active metabolic tissue and is constantly being formed by cells called osteoblasts and broken down by cells called osteoclasts. About 10% of bone is replaced each year, so that your entire skeleton turns over every 10 years.
Bone Formation and Bone Resorption
There are many sites for formation and breakdown of bone. And these sites vary in their sensitivity to hormones responsible for bone activity. Androgens, the male hormones, build up the outer, or periosteal, layer of bones; Estrogens, the female hormones stimulate growth of the inner, or endosteal, layers of cortical or compact bone (see http://darkwing.uoregon.edu/~louiso/BNSTRUC.GIF). In the long (arm and leg) bones, the thickness may be the same in men and women but because of their greater diameter, bones in males are stronger in resisting stress. These hormones add to the thickness of the bone pillars (trabeculae) in cancellous, or spongy bone that is present inside the vertebrae and at the ends of the long bones (see figure linked above.) Estrogens are active in bone formation in men as well as women, and the net thickness of trabeculae in cancellous bone will be greater in men. Because of the larger diameter of cortical bones and thicker trabeculae of cancellous bones, men have a larger bone mass than women.
Estrogens not only increase bone formation, they inhibit bone resorption by decreasing the activity of osteoclasts. When estrogen is withdrawn, bone resorption increases. The actual mechanism is a decrease in the inhibition of osteoclast formation. The increase in the multicellular osteoclasts, and the larger number of resorptive sites they occupy, creates an imbalance between formation and breakdown of bone, resulting in net bone loss. In women this is accelerated at the time of menopause with the steep drop in estrogen.In the United States, poor nutrition, or wrong nutrition, and inadequate activity make the genetic predisposition that many have for fragile bones much worse.
In the first 5-8 years of menopause, 1%-2% of bone is lost per year in addition to the 0.4% of bone lost per year after peak bone density is achieved at age 30. In women at menopause, the decline in estrogen levels leads to an increase in the lifespan of osteoclasts which break down bone and a decrease in the lifespan of the bone-forming osteoblasts. Among men, age-related decreases in estrogen also result in increased bone breakdown.
Measuring Bone Mass
The term "bone mass" simply means the amount of bone in the whole body or in a specified area of bone. We currently measure bone mineral density (BMD) as a way to estimate bone mass. From BMD measurements we have developed standards to determine the presence of osteoporosis. The techniques used include single and dual-energy x-ray absorptiometry (SXA & DXA), quantitative computed tomography (QCT) and quantitative ultrasound.
In SXA and DXA, bone mineral density is expressed as the mineral content divided by a given area of bone in two dimensions. The sites usually measured are the hip and lumbar vertebrae. DXA is currently the test used most commonly for diagnosis and treatment decisions for osteoporosis.
QCT measures density in three dimensions and can give a more accurate picture of bone density. The radiation exposure is much higher than DXA and its value in clinical practice has not been determined.
Ultrasound can determine bone density based on the transmission of sound waves through bone. This has been used on the heel bone as a screening test. DXA and SXA can also measure BMD at the heel. These peripheral measurements are less expensive than hip and spine DXA, but there is more variation in the results compared to the hip and spine measurements.
Recommendations and Risk Factors
The U.S Preventive Services Task Force recently (2002) issued a guideline that all women over age 65 be screened for osteoporosis. They based this guideline on evidence that BMD measurements accurately predict the risk for fracture and that treatment of women without symptoms of osteoporosis reduces the risk for fracture in the future. They also recommended screening 60-year-old women who have risk factors for osteoporosis. The risk factors to be considered are low body weight, weight loss, family history, smoking, alcohol or caffeine use, low calcium and vitamin D intake. (http://www.ahrq.gov/clinic/uspstf/uspsoste.htm) The National Osteoporosis Foundation also recommends screening postmenopausal women who have had a fracture.
When you visit your doctor for a check-up, certain symptoms and signs, as well as physical examination findings, may indicate that you have osteoporosis:
History and Physical Exam
Chief Complaint:You tell the doctor you think your back is becoming humped. If you notice a back deformity you have a strong chance of having osteoporosis of the spine.
Fracture: wrist or other fracture not due to major trauma in a postmenopausal individual.
Family History: As mentioned before, there are strong genetic determinants of bone density, so a family history of osteoporosis, particularly if your mother had a hip fracture increases your risk. There are racial differences in bone density. Asians have a lower bone density than whites. On the other hand, African-Americans have higher bone density.
Surgery: Hysterectomy and oophorectomy, especially before menopausal age (50s). Gastrectomy will interfere with calcium absorption.
Habits: Both cigarette smoking and excessive alcohol are associated with the development of osteoporosis.
Exercise: Lack of weight-bearing activity, particularly if combined with low weight. Conversely, excessive exercise combined with very low body fat and amenorrhea.
Diet: Low calcium and vitamin D intake. Eating disorder.
Medications: Corticosteroids, anticonvulsants, heparin, cyclosporine, aromatase inhibitors. Medication for hyperthyroidism.
ROS: Malignancy of the bone or marrow; chemotherapy, especially leading to premature menopause or gonadal insufficiency.
GI symptoms: Diarrhea may indicate celiac disease or lactose intolerance.
Musculoskeletal: Back pain. Weakness. Falls. A fracture, especially from low trauma, and especially after age 50.
Physical Exam
Physical measurements: Standard weight and height and a few physical maneuvers can alert you to risk or show evidence of developing osteoporosis. Weight of less than 60 kg or 132 lb and especially weight less than 52 kg or 112 lb.
Height: Tell your doctor if you notice that you are getting shorter. Your doctor may find a decrease in height comparing current height with previous measurements.
Two simple tests for physical evidence of vertebral fractures are:
- Wall-Occiput Distance: Inability to touch the back of your head (occiput) to the wall when standing with back and heels against the wall;
- Rib-Pelvis Distance: Your stand with your arms outstretched and parallel to the ground, as your doctor measures the distance between the lower border of your rib cage and the top of your pelvis in the mid-axillary (below armpit) line. A distance less than two fingerbreadths could be a sign of vertebral fracture.
A good screening test for motor strength, coordination and balance is the "Get-Up and Go" test. The doctor asks you to rise from a chair, walk a few yards, turn abruptly and walk back. Using the arms to rise from the chair denotes diminishing motor strength, as does a slow speed of walking. The abrupt turn tests balance and coordination.
Head and neck: Your teeth. A tooth count of fewer than 20 teeth reflects a significant loss of bone supporting the teeth and is a clue to underlying osteoporosis.
Using Bone Mineral Density Tests for Diagnosis and Therapy
Most standard DXA tests are of the hip and the spine, the first lumbar vertebra, L1, to L3 or L4, listing the values for each vertebra and the total spine. The test results usually come with an alarming display of columns of numbers, percentages, scores and a graph. The graph plots the values and standard deviations of BMD against age, that is, how different you are from the normal values for your age and sex. The norms for a population of African-American men or women will be different from those of white men or women. On the graph will be an "x" showing you where your value falls. If you get both hip and spine, you will get a different graph with numeric values for each site.
The T and the Z scores: These scores are reported as percentages of two different norms. The T score compares you with a population of young adults of your race and sex at the time of attainment of peak bone mass for that group, generally around age 30. The Z score compares you to a population of adults of the same age. Since adults have steadily decreasing norms of BMD after the third decade, you can see that the Z score for a 65-year-old may be quite normal compared to other 65-year-olds, but when you look at T score you will find it to be much lower, because it is now being compared to 25-45 year-olds. These scores are expressed as percentages of the norm. We look at the T scores because that compares you with the theoretical peak bone density of the young adult.
Figure 1.
Changes in Bone Mineral Density Over Time.
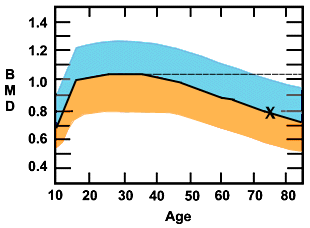
The vertical axis is the bone mineral density and the horizontal axis is age in years. The blue portion is two standard deviations above, and the orange is 2 SDs below the median in a population of white women. A standard deviation refects how far a particular value is from the average. So, in this case, at 2.5 SDs above only about 2% of a group share this value and at 2.5 SDs below only 2% of the group share this value. In other words, if your value on the test falls in either of these areas on the graph, your score is different from 98% of the sampled population. Note the sharp upsurge in the teenage years, the leveling off and peaking around age 30, and the gradual decline that increases at age 50, the time of menopause. The dotted line extending from the 30-year-old median peak, is the T score line. The "x" marks the BMD measurement of a 75-year-old woman at the median for her age. Her Z score would be 100% but her T score would be osteoporotic, 2.5 standard deviations below the young adult peak.
The World Health Organization has determined that a T score of minus 2.5 will define osteoporosis.3a That's 2.5 standard deviations below the young adult norm for your sex and race. This level has been set to enable bone density comparisons between populations and is not meant to dictate treatment. However, T scores in this range do define a population at risk for fracture that has been shown to benefit from treatment.
Special Notes About Interpretation of BMD Values
Different machines may use different populations, even of the same race and sex, for their standards, so you must use the same type of test and the same type of machine for comparative measurements over time.
Bone Markers
A number of substances are released into the circulation during the processes of bone resorption and formation that can be measured and used to mark the progress of treatment. Because there are so many variables contributing to the values of these markers, they are not used for diagnosis. The markers are classifed as resorption markers or formation markers.Currently, the most available and reliable marker for resorption is the urinary N-telopeptide, NTx; and the most available and reliable formation marker is the serum osteocalcin.
Currently there are no definitive guidelines on the use of bone markers because of the tremendous variability in the values in a single patient and among patients in a single group. Values may vary with age, sex, season of the year and time of day the specimen is taken. Young children and adolescents normally have very high levels, especially of formation markers. Secretion of markers tends to peak in the early morning hours. Food intake and kidney function will affect levels. When you evaluate the results of a marker test, it must be compared to standardized tables for your age and sex. Taking two baseline specimens under identical conditions improves accuracy.
Nevertheless, there are several reasons why your doctor might order a test for a bone metabolism marker. The marker will show the effect of treatment much faster than bone density measurements, which require two years of an intervention to register a significant change. A second reason is to determine whether you have high or low bone turnover. High levels of both resorption and formation markers, as compared to standards, indicate high bone turnover.
Improving Bone Strength and Preventing Fragility Fractures
There are three areas you must consider to improve bone strength: dietary intake, physical status and activity, and pharmacotherapy.
Diet: Intake of building blocks and deleterious substances.
Deficits in calcium intake: Adequate calcium and vitamin D are essential for growth and maintenance of bone. You must be sure they are included in your basic daily intake. They are also required for success in any kind of pharmacotherapy whether the mechanism for building new bone is by increasing formation or stopping resorption. Postmenopausal women should ingest 1200-1500 mg of elemental calcium daily; other groups, 1000 mg. Many surveys have shown that the average calcium intake is around 600 mg and is inadequate. The main sources of calcium in the western diet are dairy products. Leafy green vegetables, fish with bones, and products fortified with calcium are also good sources. Patients with lactose intolerance or with malabsorption, notably undetected celiac disease, may be particularly susceptible to low calcium absorption. If you are unable to eat/drink the recommended calcium amount in the daily diet you can take supplements.
Vitamin D intake: Adequate vitamin D is required for optimal calcium absorption. Vitamin D also improves muscle function, probably through its effect on muscle protein synthesis. Higher vitamin D intake has been significantly associated with a reduction in the number of falls among older people. The RDA of 400 IU of Vitamin D may not be adequate for the elderly, so supplementation to 800 IU is recommended for that age group.
Alcohol and caffeine: High intakes of each of these substances are risk factors for OP.
Smoking: Another risk factor.
Exercise and Activity: Bone growth is stimulated by physical stress. Life-long weight-bearing exercise is the best insurance for building peak bone mass and preventing critical age-related decline. Activities in the upright posture — walking, running and jumping — are most effective.
Falls: Many factors contribute to falls. In addition to sedentary lifestyle and poor conditioning, you may have problems with balance and vision. Medications that decrease alertness and coordination, or lead to postural hypotension and hazards around the home can all cause falls. Advancing age increases the risk that a fall will result in a fracture, not only because of increased bone fragility, but as the result of decreased muscle mass and coordination. Medical causes (e.g., cardiac, neurological disease, excess medication) need to be treated. If home hazards are present, they need to be corrected. You should engage in exercises that build muscle strength and improve balance and coordination. Specific interventions can all decrease the risk of falling and lessen the consequences.
Pharmacotherapy (In Order of Appearance)
Estrogen
Estrogen stimulates bone formation and inhibits bone resorption. The Women's Health Initiative showed decreased hip and vertebral fractures in patients taking estrogen. Estrogen increases bone density during the time of treatment but as soon as estrogen is stopped bone density starts decreasing. Because the Women's Health Initiative did not show the protective effect against heart disease that we had assumed was operative and because of the increased incidence of breast cancer, estrogen is no longer recommended for first-line prevention of osteoporosis. It may be used with careful monitoring for OP treatment if nothing else helps.
Calcitonin (Miacalcin Nasal Spray or Injection)
This protein derived from the parathyroid glands modulates serum calcium levels by inhibiting resorption, primarily at vertebral sites. This action is mild compared with other antiresorptive agents. No study has demonstrated a significant decrease in fracture risk. Calcitonin has the interesting effect of decreasing the pain of recent vertebral fractures.
Calcitonin must be given by injection or as a nasal spray. The preparation mostly used for osteoporosis is Miacalcin Nasal Spray in a dose of 200 micrograms daily, delivered by one activation of the nasal spray. The main side effect is nasal irritation. Allergic reactions can occur but are uncommon.
The Selective Estrogen-Receptor Modulators (SERMs)
Estrogen-like compounds that have differing effects on the sites of estrogen action have been developed. Tamoxifen does have a weak effect on bone and causes an increase in bone density. Raloxifene (Evista) was specifically developed to treat osteoporosis and has a stronger effect on bone, midway between estrogen and tamoxifen. So far, studies have shown that raloxifene decreases vertebral fracture incidence but not hip fractures. Raloxifene does not produce unwanted effects on the uterus, so avoids the problems of tamoxifen, and also decreases the incidence of estrogen-positive breast cancer. Raloxifene may increase hot flashes and venous thrombosis. Other SERMs are currently being developed, so stay tuned.
The Bisphosphonates: Alendronate, Risedronate and Ibandronate
These compounds bind to the active resorption sites in bone and inhibit the action of osteoclasts that break down bone cells. Both alendronate (Fosamax) and risedronate (Actonel) have been shown to increase bone density and reduce fracture rate at both vertebral and nonvertebral sites compared with placebo. Both are oral preparations and can be taken for prevention or treatment of OP. Although initial studies were on daily dosage, further research has now shown that both drugs can be taken weekly. This is fortunate because bisphosphonates can cause GI irritation, especially in the esophagus. They can cause esophagitis or esophageal ulceration, particularly if the pill gets retained in the esophagus or stomach juices containing the drug get washed back up into the esophagus. Patients should take their medication on an empty stomach, first thing in the morning, followed by a full glass of water and take nothing else by mouth, staying in an upright position for at least one-half hour. Bone and muscle pain and eye inflammation have also been reported but are infrequent.
The dosages of alendronate are 5 mg/day or 35 mg/week for prevention and 10 mg/day or 70 mg/week for treatment of OP. For risedronate the doses are 5 mg/day and 35 mg/week for both indications.
The new kid on the block is ibandronate (Boniva), approved in 2005 for a daily dose of 2.5 micrograms or a monthly dose of 150 micrograms. It has the same GI side effects as the other bisphosphonates but monthly exposure will decrease the risk and frequency of side effects. Rare cases of eye inflammation have been observed but not the severe bone, joint and muscle pain.
Zoledronate, an intravenous bisphosphonate used for hypercalcemia and malignancies, is now being tested as a once-a-year treatment in postmenopausal women.
Parathyroid Hormone (PTH)/Teriparatide (Forteo)
Teriparatide is the portion of parathyroid hormone (PTH), which is biologically active. PTH can either break down or build up bone, depending on the type of exposure. Continuous infusion of PTH or chronic exposure to elevated levels of PTH, as in hyperparathyroidism, increases bone breakdown. On the other hand, intermittent exposure, as in a daily dose, increases bone density and strength.
Teriparatide must be administered by injection. The dose is 20 micrograms subcutaneously every day. The FDA has put a limit of two years on treatment because osteosarcoma was seen in growing rats given high doses of the drug for two years. No cases have been seen in humans given the drug or in humans with hyperparathyroidism.
Patients taking this medicine need to be cautioned about orthostatic hypotension (low blood pressure upon standing), which has been seen in some patients after the first few doses of the drug. Patients must be taking adequate calcium and vitamin D when on teriparatide because of its strong action on bone formation.
Cost is an issue with teriparatide — more than $500/month compared with $60-$70/month for raloxifene and the bisphosphonates.
Some Observations About the Pharmacotherapies
I think you can see from the above discussion that in the last 10 years we see osteoporosis pharmacotherapy transformed and improved. We now have three bisphosphonates, one SERM and parathyroid hormone. We have learned a great deal about how all the OP drugs work, separately and together, and we need to change our thinking about some drugs we used before. Let me give you a quick run-down.
Estrogen can no longer be considered a first-line drug for either prevention or treatment of postmenopausal osteoporosis (PMOP). While a woman is using estrogen in the immediate menopausal period, she will not have that sharp drop-off of BMD but we now know that when estrogen is discontinued, the drop in BMD will occur. Any woman over 65 and any woman younger than 65 with OP risk factors who is discontinuing estrogen should have a BMD test. If osteoporosis is present, alendronate would be a good choice because it has been shown to sustain bone density after stopping estrogen. It counteracts that increase in resorption that occurs with estrogen withdrawal.
Calcitonin should also be considered a second-line drug. The bisphosphonates, SERMs and PTH are all more effective and are backed up by strong evidence. Calcitonin's analgesic effect on painful vertebral fractures can be a helpful adjunct in some patients.
Alendronate (Fosamax) has been available in the U.S. for nearly 10 years, and a study reporting on 10 years of treatment with the drug showed increasing bone mineral density in vertebral sites and stable BMD at other sites. During the five years after treatment was discontinued, BMD decreased slowly. Because the bisphosphonates are incorporated into the bones, there has been a concern that over time the bones might become more brittle. This effect has not been seen in these recent observations, which is somewhat reassuring.
How do the drugs compare? PTH causes the most gains — 8% per year in the spine compared with 3-4% per year by alendronate. Raloxifene is in about the same range as the bisphosphonates.
Because PTH increases bone formation and bisphosphonates stop resorption, will using both together result in greater gains in bone strength? It turns out that the effects are not additive. BMD gain with a combination of PTH and alendronate was midway between gains by each drug separately, PTH causing the greatest gains. On the other hand, using the drugs sequentially is advantageous. Alendronate sustains bone density after the withdrawal of estrogen or parathyroid hormone treatment.
Using Bone Mineral Density and Bone Markers to Aid Therapy
Bone density changes, as measured by DXA, are only truly significant after two years of treatment. Markers, however, can show a significant change in 3-6 months. This reassurance can be particularly useful in severely osteoporotic patients who are at high risk for fracture. For such individuals, it is better to find out sooner, rather than later, that they are not responding to or not complying with the treatment. When the bisphosphonates first came out in daily dosage form, noncompliance was frequent because of the inconvenience of dosage and high risk of GI side effects. Many prescriptions were not filled or refilled.
Another use of markers is to determine whether a patient with osteoporosis has high bone turnover or low turnover. Someone with high turnover (high values of both resorption and formation markers) is a good candidate for anti-resorptive medications. A person with low turnover would not be expected to improve bone formation by slowing resorption, since resorption is low to begin with and resorption and formation are coupled. That patient would be a candidate for teriparatide, which stimulates formation.
Summary
Osteoporosis is a silent disease. You may not be aware you have it until you sustain a fracture or have a bone density test. Yet osteoporosis may be prevented by good dietary and exercise habits in adolescence and young adulthood to achieve a high peak bone mass, and maintainance of those habits to slow the loss of bone mass after age 30. If you are diagnosed with osteoporosis you can stabilize and increase your bone strength through diet, exercise and medications.




