Dr. Shestopalov is Assistant Professor, Bascom Palmer Eye Institute, Department of Ophthalmology, Department of Cell Biology and Anatomy University of Miami Miller School of Medicine, Miami, Florida.
The lens in your eye is normally clear and enables you to see clearly. When the lens becomes clouded with a cataract the world is like a photo you didn't focus properly — everything is fuzzy and indistinct.

Courtesy, National Eye Institute (NEI/NIH)
Cataracts are the most common cause of vision loss and blindness. In the U.S. alone, more than 20 million people over 40 either have a cataract or have had cataract surgery. They develop over a period of years or decades and can be inherited or caused by an injury or caused by damage accumulated over time. The main treatment for cataracts is to remove them through surgery. There are two main surgical procedures used for this, each of them involving removing the lens and replacing it with an artificial substitute. Both of these surgeries are relatively safe and effective.
Aging and the Lens
Aging is the most common cause of cataracts. The cells of the human lens are unique. Made up mostly of water and proteins, the outer layer of the lens is able to protect itself from light damage by lowering its oxygen content, manufacturing protective substances called antioxidants, and maintaining a constant internal circulation of water, ions and metabolites.
These powerful protective mechanisms can be damaged by traumatic injury and by the effects of aging, particularly in those over 50. Aging can create a buildup in the lens of oxidized proteins and lipids (i.e., fat cells). It can also cause antioxidants to become become depleted, which in time leads to the formation of a barrier between the outer layers and the core of the lens.This is the first step in the development of cataracts, called by the ancient Egyptians, "darkening of the pupil" and "white disease of the eye."Cataracts are the most common cause of vision loss and blindness. In the U.S. alone, more than 20 million people over 40 either have a cataract or have had cataract surgery.
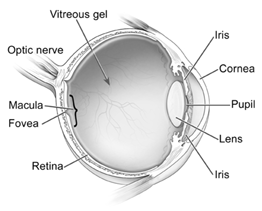
Courtesy, National Eye Institute (NEI/NIH)
The Different Types of Cataracts
Even among medical authorities, there is no commonly accepted way of classifying cataracts. Some experts classify them by appearance, color intensity or location. Others divide them into infantile (including juvenile), age-related, inherited and systemic. Of these, the age-related type is the most common.
Congenital Cataracts
Congenital cataracts occur in very young children and sometimes run in families. Although quite rare in developed countries, this type has a devastating lifelong impact on vision because they interfere with the normal development of the eye. If left untreated — either by surgery or corrective glasses — congenital cataracts can cause amblyopia (lazy or crossed eyes), squint, nystagmus (fluttering or other involuntary eye movement), and even blindness. Prevention of this kind of cataract is an important component of the World Health Organization's (WHO) international campaign for the elimination of avoidable blindness by the year 2020.
Congenital cataracts are caused by genetic mutations that take place before birth, in the developing fetus. The genes that cause hereditary cataracts have recently been mapped and identified. Increasing knowledge of the genetics underlying cataracts may also help us better understand the role played by environmental and nutritional factors.
Environmental Causes of Cataracts
Environmental cataracts can be caused by exposure to naturally-occurring radiation (such as sunlight or radioactivity), injury, electric shock or anything that that damages the lens capsule, lens cells or their membranes. Toxic or drug-induced cataracts are often a side effect of treatment with corticosteroids and some other drugs. Other risk factors include exposure to the rubella virus (in children); eye diseases such as glaucoma, uveitis, retinitis pigmentosa, ischemia, retinal detachment and intraocular tumors; and diabetes.
Age-Related Cataracts and Oxidation
The biggest environmental risk factor for cataract formation is aging. Aging makes the eye vulnerable to processes called oxidation and oxidative stress, which damage the proteins in the lens and impair the lens's ability to protect itself. Recently, medical science has made significant strides in understanding how oxidation causes age-related cataracts. In general, oxidation occurs when oxygen molecules interact with other substances, ranging from metal to fruit to human tissue. Some forms of oxidation are destructive, such as the rusting of an automobile or the spoiling of fruit. When it interacts with iron, for example, oxygen creates a slow burning process, which leaves behind the brittle brown substance we call rust. The process of oxidation depends on the amount of oxygen present and the nature of the material it touches. True oxidation happens on a molecular level; with the naked eye we see only its effects. In the case of fresh fruit, for example, the skin provides a barrier against oxidation. Once the skin has been broken and individual cells come in contact with air, oxygen molecules start burning them. The result is a type of rust that we see as brown spots.
As mentioned above, the eye does have ways of protecting itself against oxidation, including deploying its own antioxidants. This is why many people develop cataracts late in life or not at all. Remarkably, some people seem to be almost entirely protected from lens oxidation. For these lucky few, there is no significant oxidation of the proteins in the center of the lens with advancing age, even past age 80.Aging makes the eye vulnerable to processes called oxidation and oxidative stress, which damage the proteins in the lens and impair the lens's ability to protect itself.
There are three major types of human age-related cataracts; their technical names are nuclear, cortical and posterior subcapsular, the first two being the most common.
Fiber-based v. Non-Fiber-Based Cataracts
Cataracts can be divided into fiber- and non-fiber-based cataracts. In the fiber-based group, the form of the cataract is determined by the arrangement of the lens fibers, while for non-fiber-based cataracts, form is unrelated to lens fiber organization.
Fiber-based cataracts are further divided into two categories, called sutural and non-sutural. The latter are usually congenital and run in families.
Is It Time for Surgery?
Early cataract symptoms can often be taken care of by new glasses, improved lighting, anti-glare sunglasses or magnifying lenses. When these measures no longer help, surgery is the only remaining option. Cataract surgery is fairly straightforward: the surgeon removes the damaged natural lens and replaces it with a man-made lens.
A good guideline to use in deciding whether or not to have cataract surgery is to ask yourself if your vision loss is getting in the way of everyday activities such as driving, reading or watching TV. If the answer is yes, you should speak with your doctor or eye care professional. After talking through the benefits and risks of surgery, you will be able to make an informed decision about whether cataract surgery is the way to go. In most cases, there is no great rush; waiting to have the surgery will not affect the eventual outcome.
An exception to this rule is cataracts that interfere with the treatment of another eye problem, such as age-related macular degeneration or diabetic retinopathy. In this case, you may have to have cataract surgery sooner than would be justified by your symptoms alone.
Remember that not all cataracts need to be operated on.
If you need cataract surgery in both eyes, each eye will be done separately, usually four to eight weeks apart.
What Surgery Is Like
There are two types of cataract surgery:
- Phacoemulsification: A small incision is made on the side of the cornea, the clear covering on the front of the eye. The surgeon inserts a tiny probe. The probe uses ultrasound waves to soften and break up the lens so that it can be removed by suction. Most cataract surgery today is done this way.
- Extracapsular surgery: The surgeon makes a long incision on the side of the cornea and removes the cloudy core of the lens. The rest is removed by suction.
Like any surgery, cataract surgery carries risks, such as infection and bleeding. After surgery, it is extremely important to keep your eye clean, wash your hands before touching your eye, and use prescribed medications to avoid infection. Serious infection can cause loss of vision or even blindness.
After surgery, it is extremely important to keep your eye clean, wash your hands before touching your eye, and use prescribed medications to avoid infection.
Risks
Cataract surgery slightly increases your risk of a detached retina. One sign of a detached retina is a sudden increase in what are called flashes (i.e., of light) or floaters. Floaters are small specks that seem to float about in your field of vision. If you notice a sudden increase in floaters or flashes, see an eye care professional immediately. If you think it might be a detached retina, go to an emergency service or hospital right away. Remember that a detached retina causes no pain. Speedy treatment is key in preventing permanent loss of vision.
Despite these risks, cataract surgery is one of the most common operations performed in the United States. It also is one of the safest and most effective. 90 percent of people who have cataract surgery will see improvement in their vision.
A cataract operation usually takes less than an hour and is virtually painless. Many people need little or no anesthesia, other than enough to numb the nerves in and around the eye.
After the operation, you will be watched for a few hours for bleeding or other problems. Most people who have cataract surgery go home the same day.
Secondary Cataracts
Sometimes, after people have had cataract surgery, new cataracts appear; these are called secondary cataracts. Modern cataract surgery is performed by cutting out the lens and implanting a clear plastic intraocular lens (IOL) into the remaining "capsular bag." Secondary cataracts occur when left-over lens cells move under the IOL and form a fibrous opaque layer. Secondary cataracts develop in 5-15% of patients who undergo successful cataract surgery. Fortunately, they can be fairly easily corrected by laser treatment.
Can Cataracts Be Prevented?
Given the association between oxidative damage and age-related eye problems, it is not surprising that over 70 studies have attempted to relate lack of antioxidants in the diet to the risk of developing cataracts and other eye disorders. Many researchers believe that good nutrition and taking high doses of antioxidant supplements can reduce a person's risk for age-related cataracts. Observational studies suggest that a healthy lifestyle, with a diet containing foods rich in antioxidants, particularly lutein and zeaxanthin, (both found in green, leafy vegetables), as well as omega-3 fatty acids, (found in cold water, oily fish, flaxseed oil and other sources), appears to help prevent eye disorders, possibly including cataracts.
However, even the most potent antioxidants cannot actually cure a cataract. And the science on the effectiveness of supplements is inconclusive. Recently, the FDA concluded that no firm proof exists for health claims about the intake of lutein or zeaxanthin. Another study concluded that a multivitamin-multimineral supplement with a combination of vitamin C, vitamin E, beta-carotene and zinc (with cupric oxide) is effective in reducing the risk of cancer, but does not recommend it for cataracts. On the other hand, there is certainly no down side to eating a healthy diet with lots of green vegetables.
So, what can we do if we are concerned about age-related cataracts? A healthy diet and common sense about sun exposure (wear sunglasses and a hat with a brim to block ultraviolet sunlight) seem to be the best bet to delay or prevent cataracts.
We can expect to see better methods of cataract prevention and therapy in the near future as we learn more about how to protect the machinery of the lens from damage from oxidation, injury, toxicity and other factors and how to correct genetic defects. In the meantime, the best weapons we have today in the battle against cataracts are: taking antioxidants either in the form of antioxidant rich food or in the form of supplements; cautious use of steroids and other drugs; and improved eye surgery.
ADVERTISEMENT




