PCP is caused by a normally harmless organism that is widespread in the human body. Until then, it was known to cause disease only in people whose immune systems had been weakened, usually by cancer or cancer treatments. The men in the CDC report, however, did not have cancer or any other known health problem. CDC experts concluded they were seeing something new, which they called "cellular-immune dysfunction related to a common exposure," and characterized as "a disease acquired through sexual contact."
As other similar case reports came in, risk groups were defined: gay men, Haitians, IV drug users. Tests that measured victims' cellular immunity told the same story over and over again: loss of T-lymphocyte cells, which are important players in the human immune system, and poor lymphocyte response to infections. Soon afterward, other associated illnesses and conditions were identified, including lymphadenopathy, or swollen lymph nodes; Kaposi's sarcoma; and various fungal and parasitic diseases.
In January 1983, the CDC reported on two women with impaired immune systems who were sexual partners of men with AIDS. One was a 37-year-old African American woman with thrush (oral candidiasis), lymphadenopathy (swollen glands) and PCP. Blood studies showed lymphopenia (low levels of lymphocytes in the blood) and undetectably low levels of T-helper cells, another sign of a severely impaired immune system. Her steady male sexual partner for the previous six years had been a man with a history of IV drug use who had died of AIDS in November of 1982. The second case was a 23-year-old Hispanic woman, also with lymphadenopathy, lymphopenia, and decreased T-helper cells. Her steady sexual partner was a bisexual male who had developed AIDS symptoms in June of 1982: lymphadenopathy, oral candidiasis, PCP, and Kaposi's sarcoma.
Twenty years later, these two women remain typical of the largest subgroup of women with HIV/AIDS in the U.S. today: members of a racial or ethnic minority who acquired the disease through heterosexual transmission from a bisexual or IV drug-using partner. Second in size to this group is the subgroup of women with HIV/AIDS who are themselves IV drug users.
A Virus That Does Not Discriminate
AIDS entered the United States primarily through the gay male population (the current scientific term is "men having sex with men," or MSM). In the beginning, some thought the disease affected only gay men. It did not take long for it to become clear that AIDS was caused by a nondiscriminating virus, first called human lymphotropic virus type III/lymphadenopathy associated virus (HTLVIII/LAV) and later renamed human immunodeficiency virus type 1 (HIV-1). This was a disease that would infect and kill anyone if the circumstances were favorable. One favorable circumstance was transmission from one IV drug user to another through a shared hypodermic needle. Another was transmission through heterosexual sex.
What Should We Call It?
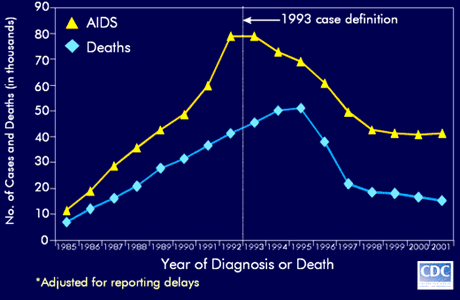
Before the virus causing AIDS was identified, the CDC created what is known as a "surveillance definition." This is a provisional definition made for the purpose of gathering information about a new disease. In the case of HIV/AIDS, the original surveillance definition included constitutional symptoms; neurologic conditions; opportunistic infections called by viruses, bacteria, fungi and parasites; and cancers. As with other surveillance definitions, it was revised as new data came in. In 1992, the 1987 definition was expanded. This led to a sharp peak in the incidence curve, as shown in Figure 1 below.
Figure 1.
Estimated Incidence of AIDS and Deaths of Adults and Adolescents with AIDS*, 1985-2001, United States.
Some time after the virus was identified, infection with HIV was distinguished from AIDS, the critical point at which the virus has destroyed immunity to the extent that the infected person is no longer able to fight off certain infections.
The first step in treating HIV/AIDS was an effort to control these "opportunistic" infections, but soon specific anti-HIV drugs, the antiretrovirals, were developed. These have transformed an infection that was essentially a death sentence into a manageable chronic illness. With the arrival of these medicines in the mid-1990s, the AIDS epidemic changed dramatically. The statistical incidence of AIDS decreased as fewer cases of HIV progressed to AIDS, and with AIDS patients living longer, the death rate from AIDS dropped (Figure 1). Finally, the prevalence of AIDS increased because people with AIDS were living longer.
Special Note
Before continuing with this discussion of HIV/AIDS in women, a distinction in the statistics should be noted. Now that we have identified the virus causing AIDS, HIV-1, we have statistics on individuals diagnosed with HIV, as distinguished from individuals diagnosed with AIDS. HIV cases change into AIDS cases when the disease progresses. On the other hand, not all AIDS cases are first diagnosed with HIV. So just remember that HIV and AIDS statistics do not represent the same people. The term "infected with HIV," however, refers to those with HIV and AIDS, combined.
Women Not Excluded
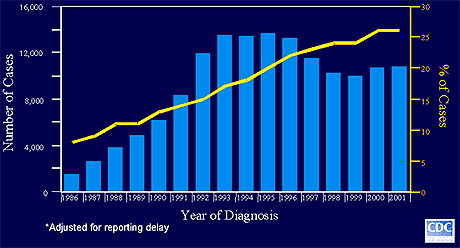
Although most of the cases reported early in the epidemic were men, it was not long before AIDS in women was identified. Women contracted the disease primarily by sex with bisexual men or infected drug-using men or through sharing contaminated needles with infected injection drug users (IDUs). The proportion of all AIDS cases that were women and adolescent girls (aged >13 years) increased from 8% in 1986 to 26% in 2001 (Figure 2).
Figure 2.
Estimated AIDS Incidence in Women and Adolescent Girls.
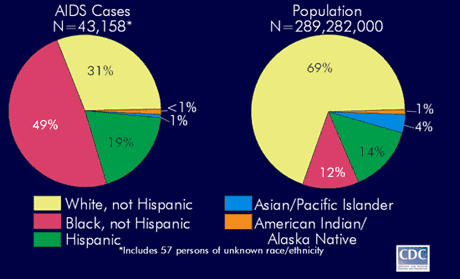
AIDS cases continue to be concentrated in racial and ethnic minority groups. In 2001, 49% of AIDS cases were African Americans. African Americans make up 12% of the U.S. population.
Figure 3.
Reported AIDS Cases and Estimated Population by Race/ethnicity, 2001.
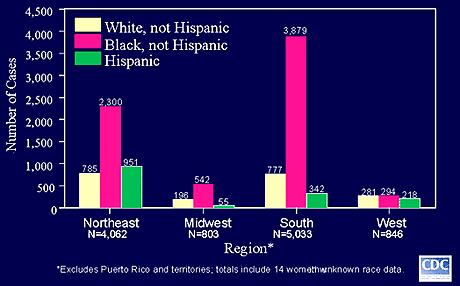
More than 75% of women with AIDS and HIV belong to racial or ethnic minorities, African American or Hispanic, and more than 50% of new infections are in African American women. This concentration is particularly pronounced in the South.
Figure 4.
AIDS Incidence Among Women and Adolescent Girls by Region and Race/ethnicity, 2001.
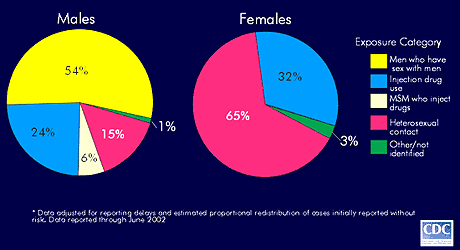
Initially, intravenous drug use was the most common mode of transmission to women, but, in 1991, heterosexual contact with an infected person became the most common mode. In 2001, 65% of women with AIDS contracted the virus through heterosexual contact, whereas 15% of men reported heterosexual transmission.
Figure 5.
Estimated AIDS Incidence Among Adults and Adolescents by Sex and Exposure.
Heterosexual Transmission
An infected man is twice as likely to transmit HIV to a female partner as the reverse. Anal sex carries a higher risk for infection than vaginal sex. Damage to tissues, such as microtrauma during sex and preexisting genital ulcer disease, increases the rate of transmission. Genital ulcer disease can increase the risk of transmission 1.5 to 7-fold. A gynecological conditon called cervical ectopy is also associated with increased risk. Sex during the menstrual period increases risk. A partner is more likely to pass on the infection if he or she has acute or primary HIV infection or more advanced disease with a higher viral load or a lower CD4 count.
Primary HIV Infection
The first symptoms of HIV infection are very much the same in men and women, although they may be more pronounced in women. They are similar to those of other acute viral illnesses: fever, joint pain, muscle ache, diarrhea, vomiting and lymphadenopathy. Weight loss, sore throat, rash and oral ulcers are also common.
Asymptomatic HIV
Those with HIV infection may live in apparent good health for as long as 10 years, until cell-based immunity is destroyed to a critical point. AIDS-defining illnesses then begin to appear, as CD4 cell counts continue to fall in untreated patients. The decision to begin treatment is usually based on HIV RNA levels (i.e., viral load) and CD4 counts.
Nearly one million people in North America are infected with HIV, and an estimated quarter of these people are not aware that they have the infection. More than one fourth of the 45,000 newly diagnosed cases every year are women. Better detection of HIV in women could be achieved through closer attention to the risk factors for contracting HIV infection and the diagnostic clues that might be seen during a check-up or other examination.
Any woman who goes to the doctor should discuss any high risk behaviors with their health care practitioner. These behaviors include:
- Multiple sex partners
- A partner with an HIV risk, such as intravenous drug use or bisexual lifestyle
- A sexually transmitted disease
- Trading sex for drugs or money
- Personal use of injection drugs or non-injection drugs such as crack cocaine or methamphetamines
Some illnesses should immediately arouse suspicion of an underlying HIV infection. One example is herpes zoster in a healthy person under the age of 50 or thrush not related to recent antibiotic use. In women, conditions such as recurrent vaginal candidiasis, cervical dysplasia, HPV (human papilloma virus), or cervical cancer can be manifestations of underlying HIV.
If a woman tests positive for HIV, CD4 and viral load tests are used to determine the degree of immune damage and need for treatment. HIV viral load is used to monitor response to therapy, while CD4 counts are used primarily to assess the risk for opportunistic infections. In primary HIV infection, viral load is generally very high and infected persons are at a high risk to transmit the infection to others. There are some sex specific differences in viral loads, with some studies showing a lower viral load in women than in men when the CD4 counts were the same.
AIDS Defining Illnesses
Initially AIDS was diagnosed by the appearance of unusual infections that invade a body with weakened cellular immunity. PCP, caused by a parasite, and Kaposi's sarcoma, caused by a newly identified virus, and human herpes virus 8 were some of the first to be identified. The revised classification of 1993 added cervical cancer to the list. This highlighted the fact that AIDS defining illnesses can be different in men and in women.
In one study, the most common initial manifestations in women were recurrent candida vaginitis (37%), lymphadenopathy (15%) and bacterial pneumonia (13%). Of the AIDS defining illnesses, Kaposi's sarcoma, seen in 40% of homosexual men and 11% of heterosexual men, was only 1.8% in women. Esophageal candidiasis occurred in 34%, PCP in 20% and mucocutaneous herpes simplex virus in 18% of women with HIV.
Human Papillomavirus (HPV) Infection and Cervical Cancer
In the revised surveillance definition of AIDS published at the end of 1992, invasive cervical cancer was added to the list of AIDS defining diseases. Higher numbers of HIV-infected women are infected with human papillomavirus (HPV), especially the oncogenic, or cancer-causing, strains. Coinfection with HIV and HPV is associated with more high-grade cervical dysplasia, a pre-cancerous condition, and more rapid progression of dysplasia to cervical cancer. In women with greater degrees of immunosuppression and a higher viral load, the prevalence of dysplasia increases.
The CDC has recommended that HIV infected women have Pap smears six months apart for two screenings. If the results are normal, annual screening should be done. A study evaluating the effectiveness of this intervention compared with more aggressive regimens found the CDC regimen to be both effective and cost-effective.
HIV and Pregnancy
HIV/AIDS is a disease of young adults, and as the AIDS epidemic spread into the female population in this country, HIV in pregnancy became a major issue. Today, an estimated 5,000-7,000 HIV-infected women in the U.S. give birth every year. Before medical interventions were developed, transmission from mother to child occurred in 20-30% of pregnancies. In addition, 8-20% of breast fed babies became infected through their mother's milk. One third of transmissions associated with pregnancy were estimated to occur during pregnancy and two-thirds during delivery.
Initially, careful obstetrical precautions through the course of pregnancy and during delivery were the only weapons available to prevent this. Now two other factors have evolved to help produce better outcomes: antiretroviral drugs and technology allowing for measurement of CD4 lymphocyte count and, more particularly, viral load, which indicate the severity of infection and the likelihood of transmission.
Antiretroviral Therapy and Pregnancy
In 1994 the Pediatric AIDS Clinical Trial Group (PACTG) study showed that use of the drug zidovudine (ZDV) decreased mother to child transmission of HIV by 66%. The ZDV regimen consisted of oral ZDV during pregnancy, intravenous ZDV during delivery, and oral ZDV to the infant for six weeks after delivery. Combination antiretroviral therapy (known by the acronym HAART) given to mothers during pregnancy has reduced transmission further. This treatment became available in 1996.
A study in the U.S. started in 1990, and followed for several years, measured transmission in various treatment groups as follows: no antiretroviral treatment: 20%; ZDV alone: 10.4%; combination therapy without protease inhibitors: 3.8%; and combination therapy with protease inhibitors: 1.2%.9 Now with increasing use of HAART, women who are already on antiretroviral regimens are becoming pregnant. Studies are underway to evaluate the safety of the new drugs for mother and fetus.
Viral Load and Vertical Transmission
Higher viral load early in pregnancy and at delivery are both associated with higher risk of transmission. Now the goal of therapy is to reduce viral load to undetectable levels. While the risk of transmission is very low when maternal viral load is undetectable, transmission to the newborn has been known to occur at all viral load levels. Viral load is now measured at 34-36 weeks to give time for counseling and decision-making about the mode of delivery.
Obstetrical Management
Except in women with very advanced disease, HIV has little effect on pregnancy outcomes and pregnancy has not been shown to affect the course of HIV. During pregnancy, any invasive obstetrical procedure, such as amniocentesis, should be avoided. Other sexually transmitted diseases (STDs) should be detected and treated, especially those that produce genital ulcers.
Exactly how transmission occurs during the course of pregnancy is unknown. We do know that a placental infection can breach the placental barrier and allow infected lymphocytes or virus into the fetus. However, this is not a common complication and does not account for most of the cases. Transmission may occur by the same mechanism without placental infection and there may be other ways for the virus to access fetal circulation.
One thing is certain: the amount of infection in the mother is a highly significant factor. As the severity of the maternal infection increases, so does the transmission rate.8 Intrauterine transmission is significantly decreased by antiretroviral therapy, particularly zidovudine.
Management of Delivery
As noted above, an estimated two-thirds of infections in babies occur at or around delivery. Anything that allows the mother's blood or genital secretions to contact the baby increases risk. Important precautions include avoiding invasive monitoring, artificial rupture of membranes when labor is progressing, or other invasive procedures. Premature rupture of the membranes of greater than four hours duration has been shown to increase risk.
Elective caesarean section has been offered to women in order to avoid the trauma associated with vaginal delivery. This has been shown to decrease transmission by 50 to 75%. On the other hand, non-elective or emergency caesarean section, done after the onset of labor and rupture of the membranes, does not significantly decrease transmission compared to vaginal delivery, and has twice the complication rate.
The introduction of antiretrovirals and our improved ability to measure viral load have made pregnancy management more complicated, but have allowed a fine tuning of delivery decisions to decrease the likelihood of transmission. Women receiving antiretrovirals who have undetectable viral loads and deliver vaginally have as low a transmission rate as women on zidovudine (ZDV) who have elective C-section. Currently, the American College of Obstetricians and Gynecologists recommends elective caesarean section at 38 weeks for women with HIV RNA levels of more than 1000 copies/ml at the time of delivery.
HIV and Breast Feeding
HIV is present in breast milk and is responsible for an additional 8-20% of mother-to-child HIV infections. This is a particular problem in developing countries or poor areas, where formula feeding is unavailable or very costly. The protective effects of breast milk for infants are especially important in developing countries because of higher risks of neonatal infectious diseases and malnutrition.
In the U.S., HIV positive women should be counseled about the risk of transmission associated with breastfeeding and advised not to breastfeed.
Public Health Considerations and HIV/AIDS in Pregnancy
In July 1995, the U.S. government (USPHS) issued recommendations for universal prenatal HIV counseling and HIV-1 testing with consent for all pregnant women in the United States. This meant that all pregnant women, regardless of age, ethnicity, race or socioeconomic status, were to be counseled about the risks of HIV in pregnancy and advised to have an HIV test. These recommendations have been largely complied with.
A report from the Michigan Department of Health reported a decrease in perinatally HIV-infected children from 19% to 3% from 1993 to 2000. Michigan health analysts observed that HIV positive women had more STDs, alcohol and illegal drug use, and a higher rate of no prenatal care, 10% vs. 1% in women not infected with HIV. Conversely, women with no prenatal care had a lower rate of HIV testing, 58% vs. 94% in women with one or more prenatal visits. Increasing access to prenatal care and treatment for drug and alcohol use are public health priorities that could further decrease mother-to-child HIV infection.
HIV/AIDS Prevention in Women
Healthcare practitioners should be alert for the clinical clues of HIV infection, such as recurrent vaginal candidiasis, herpes simplex virus or an STD. They should, as a matter of routine, take a thorough history covering all risks, and offer testing when risks are detected. Obviously, women should be counseled about safe sex and offered help for any drug or alcohol problem.
Second, all women should pay close attention to preventive messages about HIV/AIDS. Historically, surveys of AIDS cases show that a large portion of infected women know little or nothing about their risk. With investigation, the majority were determined to have had heterosexual transmission and most of the remainder injection drug use. Women should always try to determine the HIV status of their sexual partner.
Many studies have shown that women were simply unaware of their risk and were not taking precautions against heterosexual exposure to HIV virus. Condoms should be used at all times until partner status is confirmed. Oral sex is NOT completely safe and protection should be used in the same circumstances as vaginal or anal sex. There is no such thing as an antiretroviral "morning after" pill to protect against HIV after risky sexual behavior.
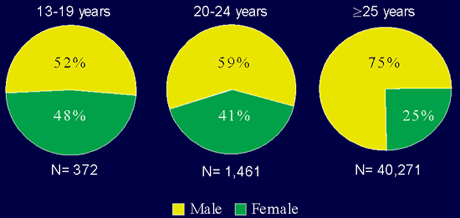
There is an ominous trend both in AIDS cases and HIV diagnoses among adolescents and young adults in the U.S. The sex ratio is moving toward 1:1. For 2001 data showed that of AIDS cases diagnosed in 13-19 year-olds, 48% were female; in 20-24 year-olds, 41% were women; and in age 25 and over, 25% were women (see Figure 6).
Figure 6.
AIDS in Adolescents and Adults By Sex and Age at Diagnosis 2001.
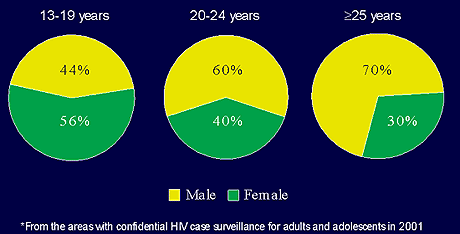
In HIV diagnoses in 13-19 year-olds, 56% were female; ages 20-24, 40% were women; and age 25 and over, 30% were women (Figure 7).
Figure 7.
HIV in Adolescents and Adults By Sex and Age at Diagnosis 2001.
In the two younger groups, 66% contracted AIDS through heterosexual contact. Three quarters of these young women are African American or Hispanic. The trends in these age groups are a harbinger of the continuing epidemic. Risky sexual behaviors and drug use continue to occur in adolescents and young adults, and need to be addressed by comprehensive educational programs.
Summary
Knowledge about the growing number of HIV/AIDS infections among women in the U.S. has been slow to sink into public consciousness. The proportion of diagnosed HIV cases in the U.S. that are women has now reached 26%. More than half of adolescents newly diagnosed with HIV infection are female. For women, heterosexual sex is the most common way of acquiring the infection, followed by injection drug use.
Use of antiretroviral drugs and viral load measurements can dramatically decrease mother to child transmission of the HIV virus. If your lifestyle places you at risk for HIV/AIDS, you need to tell your doctor so that you receive appropriate testing and timely treatment if needed. Finally, women, especially young women, must educate themselves about risk and learn to protect themselves against HIV.
Web site resources:
The CDC Divisions of HIV/AIDS Prevention. Choose health topics a-z, then AIDS/HIV. This site has comprehensive information on the U.S. AIDS epidemic: statistics, information, prevention, educational tools.
Figures: All figures in this conference were taken from the CDC public domain slide sets available on the CDC HIV/AIDS website. They are available to download for further study or educational presentations.