Statistically, males are more than twice as likely as females to suffer a burn injury. Most of these injuries happen to men in their 20s and are in some way work-related. The second most likely burn victims are young children, with liquid scalds and hot surface burns (radiators, heaters and 'potbelly' stoves) as the most common causes.
The most serious burns result from flames or scalds. About 5% of patients hospitalized with severe burns will die as a result of their injury. The majority of these are from flame burns. At least half of all people killed in building fires, however, die not from burns but rather from asphyxiation or carbon monoxide poisoning caused by fire.
Burn experts find it useful to divide burns into six major groups:
- Scalds, including immersion in or splashing by hot liquids, grease, and steam.
- Contact burns, i.e., touching a hot object or substance.
- Fires
- Chemical burns
- Electrical burns
- Radiation
Grading Burns
While this can get fairly technical, it may be useful for a victim, or friend or family member who is involved in the care of a victim, to understand the basics of how doctors grade the severity of burns. The two methods described below are the degree scale and the American Burn Association scale. Both are used as guidelines for decisions about treatment and treatment setting, for example, whether to treat a victim as an outpatient, in a hospital, or in a special burn center.
The Four Degree Scale
Even if they could not give a precise definition, most people have at least heard phrases such as "second-degree burns." Burns are graded as first, second, third, or fourth degree. When discussing these terms, it is important to keep in mind that they are somewhat subjective and that even experienced professionals commonly underestimate the severity of a burn at first sight.
As the diagram below shows, the human skin is made up of several layers. A key element of judging the grade of a particular burn is estimating how deeply — through how many layers — the burn damage goes.
Figure 1.
Cross Section of Skin.
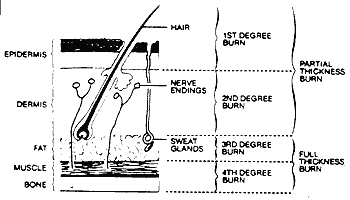
First-degree burns, the mildest type, are usually described as red, dry and painful. All but the worst kinds of sunburn fall into this category.
Figure 2.
Sunburn.
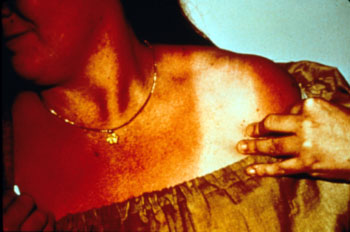 Figure 3.
Figure 3.Second-Degree Burns.
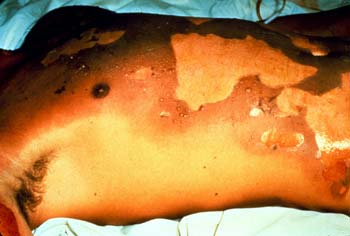
Third-degree burns are dry and leathery to the touch. The skin is numb, often white and feels hard or waxy. These burns do not heal on their own.
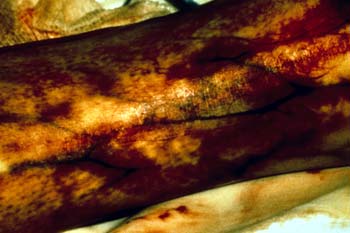
Fourth-degree burns involve the tissues beneath the deepest layers of the skin, including muscles, tendons and even bones.
Figure 4.
Deep Third- Fourth-Degree Burns.
American Burn Association Grades
When it comes to determining treatment, classification by the depth of the damage is not always the most useful way to go. For both adults and children, the American Burn Association has a method for estimating the level of care required for burns according to the percentage of total body surface area (TBSA) affected by the burn and other factors.
Minor burns - these can be managed on an outpatient basis:
- <10% total body surface area (TBSA) in an adult
- <5% TBSA in young or elderly
- <2% full thickness bur
- 10-20% TBSA burn in an adult
- 5-10% TBSA in young or elderly
- 2-5% full thickness burn
- Suspected inhalation injury
- Circumferential burn
- Associated medical problem, e.g., diabetes
- >20% TBSA burns in adult
- >10% TBSA burns in young or elderly
- >5% full thickness burn
- Known inhalation injury
- Significant burn to face, eyes, genitalia or joints
- Significant associated traumatic injury
A Special Case: Burns to Children
Even using these criteria, it can be a difficult call whether to transfer a child into a specialized care unit. Some of the factors that might lead doctors to transfer a child to a special burn unit include:
- Electrical burns
- Significant chemical burns
- Evidence of inhalation injury
- Third-degree burns over more than 5% of the body
- Second- and third-degree burns over 10% or more of the body surface area
- Second- or third-degree burns that involve the hands, face, perineum, genitalia, feet or that cross a major joint.
Treatment: Minor Burns
The first step in treating superficial burns, i.e., those without blistering or deep skin damage, is to use a lotion to insure that the skin stays moist. Antibiotics are not usually given at this point, as the skin cover is still intact and infection is not a great concern. In the case of burns which have blistered (second-degree burns), the larger blisters and those which have burst need to be debrided, or cleaned of foreign matter and dead tissue. After debriding, an antibiotic ointment, normally silver sulfadiazine, is applied.
For facial burns and people with allergies to sulfa drugs, in place of silver sulfadiazine use bacitracin or another antibiotic. These ointments are applied twice a day and recovered with a clean gauze dressing.
Another choice is the newly developed, "jelly-like" hydrocolloid dressings These dressings are left in place for about 72 hours and, after that, are changed every 5-7 days. If there is evidence of infection or excessive drainage more frequent changes may be necessary.
The reason for using antibiotic ointments, even for victims who have not yet developed any kind of infection, is that second-degree burns can seriously impair the ability of the skin to fight infection. This can make it dangerous to wait....[S]econd-degree burns can seriously impair the ability of the skin to fight infection.
Sometimes, even superficial burns will become infected. Symptoms usually occur in the first few days and include swelling and redness around the burn. The typical cause is the Streptococcus Pyogenes bacterium, which, thankfully, is treated easily with penicillin. Recently, however, more and more infections caused by Staphylococcus Aureus have been seen. This organism can be resistant to penicillin and many other antibiotics.
All burns require close follow-up for infection. If infection develops, victims may be hospitalized and given intravenous antibiotics.
For small but deep burns, the best treatment may be immediate surgery to take out and repair damaged tissue with skin grafts. This can promote and speed healing.
Finally, a very important aspect of outpatient burn treatment is dealing with the pain, which can be severe. Although many patients get considerable relief from the application of antibiotic ointment, some may need pain killing drugs or, in extreme cases, narcotics.
Treatment: Major Burns
In the first few hours after a major burn, the body experiences massive fluid shifts, which can result in profound shock if not treated. This is followed by what is called the hyperdynamic phase, as the body tries to deal with the tremendous stress and increased metabolic demands placed upon it. The victim will need immediate treatment, including adequate fluids, which can make all the difference for survival and ultimate recovery.
When a major burn victim comes into a hospital ER, treatment begins with checking the airway, breathing and circulation. An endotracheal tube may be used to maintain an open airway. If there is a serious airway blockage, a tracheotomy or other surgical procedure may be done.
For some burn victims, breathing is hampered by the presence of burns around the chest wall, which can restrict chest expansion and make breathing difficult and painful. This may be treated with an operation called an escharotomy.
An escharotomy involves cutting through the burnt tissue until healthy tissue is reached. It is usually performed with a scalpel or with an instrument heated by electricity that cauterizes damaged tissue. For burns that go all the way around arms, legs or digits ("circumferential"), escharotomies are used to save limbs by releasing the buildup of fluids that occurs underneath burned areas....[E]scharotomies are used to save limbs by releasing the buildup of fluids that occurs underneath burned areas.
As with minor burns, an important part of treating major burn victims is providing adequate pain relief.
Inhalation Injuries
Inhalation injuries, including airway damage and breathing problems, are a major cause of death from burns. These can involve the whole of the respiratory tract, from the upper airway to the interior of the lungs. There may be direct burning of the upper airway from superheated steam or gas. There may be swelling of the airway. Irritating gases may produce bronchospasm, which resembles an asthmatic attack. In time, inhalation injury can lead to pneumonia and respiratory failure.
Because these injuries do not always cause noticeable symptoms early on, doctors must watch all burn victims carefully for inhalation injuries. Inhalation injury should be suspected in anyone trapped in a building fire or who has lost consciousness during a fire. This is true especially if there was heavy smoke. Victims may have a cough, hoarse voice, or sore throat. If the injury involves the lower part of the respiratory tract, then they may have chest discomfort or pain or difficulty breathing.
Other signs of possible inhalation injury include facial or neck burns; singed hair of the eyebrows or in the nose; wheezing; or sputum that is black or sooty.
Inhalation injuries are frequently accompanied by carbon monoxide poisoning. Carbon monoxide is a substance produced by the combustion of organic material, which can be breathed in by burn victims. Doctors test for poisoning by measuring how much of a related substance called carboxy hemoglobin has reached the bloodstream. In general, a level between 0 and 10% is not dangerous. In fact, heavy smokers commonly have levels approaching 10%. Between 10 and 20% a person may experience nausea and a pounding headache. Drowsiness and an overall feeling of weakness occur at levels between 20 and 30%. Above 30%, confusion and agitation are common. Over 40% causes coma and death occurs at levels above 50%.
Besides carbon monoxide, there are also substances present in smoke that can cause breathing problems. These include benzenes, aldehydes, ammonia, acrolein and nitrogen oxide. Hydrogen cyanide is produced by burning wool and plastics.
Suspicious Burns
Sometimes, burns are warning signs of abuse. These are frequently hidden by younger victims, who will give a difficult to believe cover story, or else say that their burns were caused by themselves or by a sibling. Other possible signs of abuse are a delay in reporting or seeking treatment for the burn and a history of previous abuse.
Circular burns may be caused by cigarettes. Scald injuries are a frequent sign of child abuse. Burns that could be caused by a child being lowered into scalding water are highly suspicious of abuse.
Elder abuse may also appear in the form of intentional, circular cigarette burns.
Prevention
There are a number of risk factors that are statistically associated with burn injuries. One is low socioeconomic status. In a study from New York State, for every $1000 drop in annual income there was an increase of 49 burns per 10,000 person years. African-American children have three times the risk of suffering a serious burn than do white children. Children in single parent homes are at increased risk.
House fires are the main cause of burns to children; cigarettes are the number one cause of these fires. Parents should educate themselves and family members about the fire-related dangers of smoking, especially by elderly smokers, who are statistically more likely to smoke, as well as to have a smoking accident.
Another important prevention tool is a home smoke detector. The presence of a functioning detector has been shown to decrease the risk of death by fire by 60%. Studies show that community based smoke detector 'give away' programs also reduce the incidence of fire related injuries.
Families should also have an escape plan which is practiced regularly by parents and children. Parents should also learn about and teach 'stop, drop, and roll' techniques to their children, so that they know what to do if they should ever find their clothing ablaze.
Finally, a major cause of burns in the home is scalds from hot water taps. A good way to prevent these is to make sure your home water heater is set correctly. Experts advise that the water heater should be set at less than 120 degrees Fahrenheit (= 49 degrees Celcius). You can use a meat thermometer to gauge your hot water temperature by holding it under a running hot water tap.




