Figure 1.
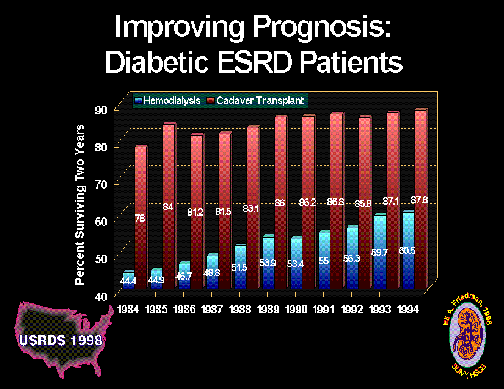
Whether treated by dialysis (combined peritoneal and hemodialysis) or a kidney transplant, survival of diabetic ESRD patients has improved continuously over the past decade. A continuing rise in absolute number and proportion of total diabetic ESRD patients is shown in the statistics provided by the United States Renal Data System 1998 Report.
Despite this progress, diabetes remains the leading cause of ESRD in all industrialized (well-fed) nations. Adequate comprehensive medical care is only infrequently given to individuals with diabetic kidney disease. Whether assessed in Europe or the US, the usual level of support for diabetic patients with symptomatic kidney disease is incomplete and often unsatisfactory.
Hemo- vs. Peritoneal Dialysis
For the large majority - over 80% - of diabetic persons who develop ESRD in the US, Europe or Japan, maintenance hemodialysis, where the patient is hooked to a machine that removes nitrogen waste products, urea and uric acid, from the blood, is the only kidney replacement regimen that will be employed. In the other technique, peritoneal dialysis, the waste products are removed during a fluid exchange in the abdominal cavity. Although enthusiasts for peritoneal dialysis for diabetic ESRD patients previously claimed survival superior to that attained by hemodialysis, careful analyses do not support such advantage.
For maintenance hemodialyis to work, a permanent and durable access to the patient's circulatory system (arteries and veins) must first be established. The most reliable variety of vascular access - an internal, surgically-made connection (arteriovenous fistula) in the wrist - is often more difficult in a diabetic than in a nondiabetic person because arteries are likely to be calcified or arteriosclerotic, that is, degraded by fatty deposits on the walls of the arteries. Many diabetic ESRD patients will need, as a result, synthetic (Dacron) prosthetic vascular grafts.
A typical hemodialysis regimen consists of three weekly treatments lasting four to five hours each. Anemia is one of the side-effects but it responds to new genetically-engineered drugs like erythropoietin which stimulates red blood cell production. Another side-effect, metabolic bone disease, caused by the loss of bone minerals, is minimized by treatment with synthetic vitamin D. Motivated patients trained to perform self-hemodialysis at home gain the longest survival and best rehabilitation afforded by any dialytic therapy for diabetic ESRD.7
Peritoneal Dialysis
Peritoneal dialysis can be successfully employed as a first choice regimen for diabetic ESRD patients. The advantages of continuous ambulatory peritoneal dialysis (CAPD) or machine sustained continuous cyclic peritoneal dialysis (CCPD) over maintenance hemodialysis include: freedom from a machine, performance at home, rapid training, minimal cardiovascular stress and avoidance of heparin, a drug that prevents clotting but, in so doing, also causes bleeding.
A typical CAPD prescription consists of four to five exchanges every day. Anemia and metabolic bone disease are managed, as in hemodialysis, with erythropoietin and synthetic vitamin D and oral calcium phosphate binders. Because it takes up so much time, CAPD can be difficult to sustain. All the studies done to date by researchers indicate that the survival of diabetic ESRD patients treated by CAPD/CCPD is inferior to that attained by hemodialysis.
No matter how sorted and analyzed, survival of diabetic ESRD patients treated by CAPD/CCPD is inferior to that attained by hemodialysis (Figs. 2-7).
Figure 2.
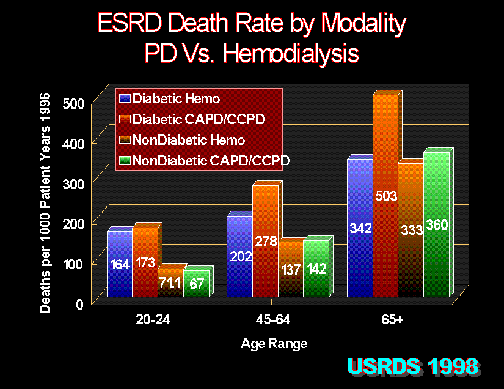
In each age group, peritoneal dialysis (CAPD/CCPD) in diabetic ESRD patients has inferior survival compared with hemodialysis. United States Renal Data System 1998 Report.
Figure 3.
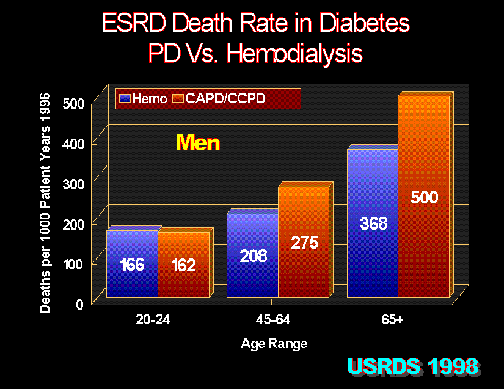
In men, peritoneal dialysis (CAPD/CCPD) in diabetic ESRD patients has inferior survival compared with hemodialysis. United States Renal Data System 1998 Report.
Figure 4.
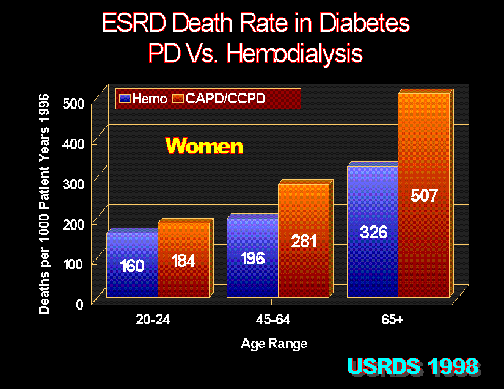
In women, peritoneal dialysis (CAPD/CCPD) in diabetic ESRD patients has inferior survival compared with hemodialysis. United States Renal Data System 1998 Report.
Figure 5.
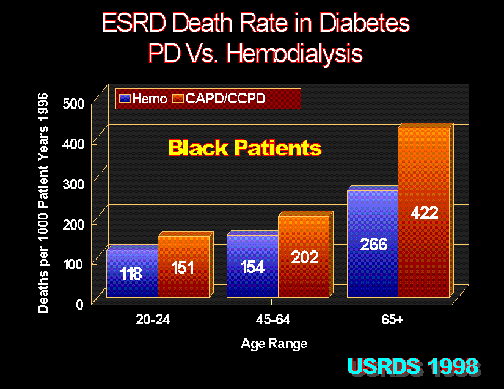
In blacks, peritoneal dialysis (CAPD/CCPD) in diabetic ESRD patients has inferior survival compared with hemodialysis. United States Renal Data System 1998 Report.
Figure 6
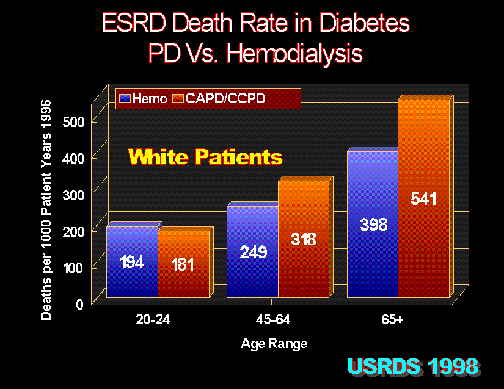
In whites, peritoneal dialysis (CAPD/CCPD) in diabetic ESRD patients has inferior survival compared with hemodialysis. United States Renal Data System 1998 Report.
Figure 7
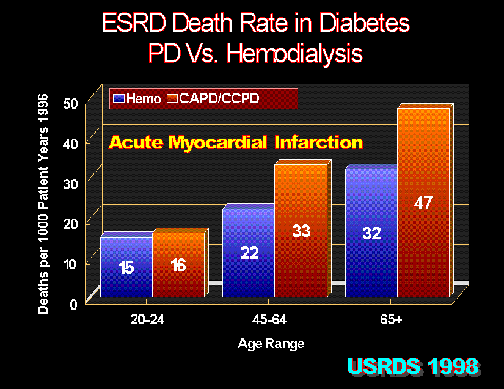
Deaths attributed to myocardial infarction (heart attack) occur at a higher rate in diabetic ESRD patients treated with peritoneal dialysis (CAPD/CCPD) compared with hemodialysis. United States Renal Data System 1998 Report.
Kidney Transplants
A functioning kidney transplant provides the diabetic patient, whose kidneys are failing, better survival with superior rehabilitation than does either CAPD or maintenance hemodialysis. Fewer than four in 100 diabetic ESRD patients treated by either peritoneal or hemodialysis will live for a decade while cadaver donor and living donor kidney recipients fare far better. More than half of diabetic kidney transplant recipients live for at least three years. Many survivors return to occupational, school and home responsibilities.
Pancreas Transplantation
A relatively new treatment, pancreatic transplantation, is growing in acceptability and technical success.
Since a defective pancreas is the source of the diabetic patient's medical problems, the consensus of kidney specialists is that the ESRD patient with Type 1 diabetes should consider a simultaneous kidney and pancreas transplant as, at least, a temporary cure of inexorable disease.
By current practice, younger patients with fewer complications are assigned to renal transplantation, while residual older, sicker patients are treated by dialysis. Combined kidney/pancreas transplants are restricted to Type 1 diabetic patients younger than age 50 who have minimal cardiac disease.
Conclusions
Maintenance hemodialysis, as performed in the U.S., does not permit return to life's responsibilities for the large majority of diabetic individuals with ESRD. The same statement is also correct for peritoneal dialysis. However, long-term survival is only attained with hemodialysis or the distinctly preferable option of kidney transplantation.




