Dr. Kevorkian is a Fellow, Division of Geriatric Medicine, St. Louis University School of Medicine. Dr. Kevorkian reports no commercial conflict of interest.
Depression in the elderly is prevalent, persistent, disabling and sometimes fatal. All of us, seniors and caretakers alike, are burdened by the myth that depression is a natural result of aging. Yes, psychiatric needs of seniors are different from those of younger persons, and the causes leading to a change in personality are different. But what's important is that many elder individuals who are depressed often go unnoticed or are not offered treatment.
It is estimated that there are 2 million people over the age of 65 in the U.S. who are depressed. Because medicine can be too focused on chronic medical illness, physicians, as a result, do not have enough time to discuss issues regarding emotional health. As our population ages, it is imperative that society and physicians become more sensitive to emotional health concerns in order to improve the total well being of elders.
- disability
- decline
- diminished quality of life
- demand on caregivers
- dementia
Family history of depression is an important risk factor for late life depression. A survey done by the National Mental Health Association in 1996 showed that 58% felt depression was a normal part of the aging process, and 49% attributed depression to personal weakness. Although depression is more common in younger patients, 20% of suicides are in older patients (highest in any age group), specifically older white men, who also had a greater rate of success of suicide. These men tended to live alone, were widowed, had chronic medical illnesses and saw their primary medical doctor a few weeks prior to suicide. Again, it is important to pay attention to the life stresses to raise awareness for suicide.
It has been shown that 50 to 70% of all medical visits by the elderly have, as a major component, emotional distress or dysfunction. These patients were less likely to have greater social contacts. They had an increasing feeling that their health was poor. As a result, they had more doctor visits and medical costs.
A study of outpatients showed that only 9% of doctors used routine questioning or screening for depression. The diagnosis of depression was made 33% of the time by formal criteria. Fifty-eight percent of doctors asked about suicide. One-third of doctors offered 5 minutes of counseling. Seventy-two percent gave medicines and 38% referred to a psychiatrist.
In the presence of chronic medical illness, physicians are less likely to discuss depression but are very receptive to patient requests for medication. Older patients tended to have depression without sadness. It has been shown that 5 to 10% of nursing home patients are depressed, as well as 11% of inpatients and 12 to 22% of nursing home patients. Loss of independent functioning has been associated with depression and the treatment of depression can improve function even when no change occurs in the medical condition that caused disability. It is also important to treat depression because, otherwise, medical burden is increased.
Since elderly patients are often dependent on caregivers, family members and doctors need to ask caregivers about their observations. Have they noticed crying spells, insomnia, weight loss, rapid emotional swings, psychomotor slowing and poor spirits? Mildly demented patients may refuse medical treatment or food and may express the desire not to live. Prompt investigation should be carried out for depression if that occurs.
For seniors, the most commonly used screen is the Geriatric Depression Scale (GDS):
Answer Yes or No to the following:
- Are you basically satisfied with your life?
- Have you dropped many of your activites and interests?
- Do you feel that your life is empty?
- Do you often get bored?
- Are you hopeful about the future?
- Are you bothered by thoughts you can't get out of your head?
- Are you in good spirits most of time?
- Are you afraid that something bad is going to happen to you?
- Do you feel happy most of the time?
- Do you often feel helpless?
- Do you often get restless and fidgety?
- Do you prefer to stay at home, rather than going out and doing new things?
- Do you frequently worry about the future?
- Do you feel you have more problems with memory than most?
- Do you think it is wonderful to be alive now?
- Do you often feel downhearted and blue?
- Do you feel pretty worthless the way you are now?
- Do you worry a lot about the past?
- Do you find life very exciting?
- Is it hard for you to get started on new projects?
- Do you feel full of energy?
- Do you feel that your situation is hopeless?
- Do you think that most people are better off than you are?
- Do you frequently get upset over the little things?
- Do you frequently feel like crying?
- Do you have trouble concentrating?
- Do you enjoy getting up in the morning?
- Do you prefer to avoid social gatherings?
- Is it easy for you to make decisions?
- Is your mind as clear as it used to be?
Depression also occurs among patients with neurologic disease — 25 to 50% of stroke patients were noted to be depressed. There was a peak at 3 to 6 months after the stroke for depression. Some patients had a spontaneous remission of their depression 1 to 2 years after their stroke. In one study, the drug sertraline reduced some of the symptoms, but not depression, as compared to the non-treated group, and in another study more depression with stroke was seen than with physical illnesses with similar disability.
It has been hypothesized that strokes in certain locations of the brain may lead to depression. Studies estimate that 10% of Alzheimer's disease patients and 20% of Parkinson's patients were depressed. According to researchers, depressed patients with Alzheimer's disease had aggression ad agitation 20% of the time, delusions 16% of the time, apathy 28 % of the time, problem behavior in 19 % of the time as well as sleep disturbance. In cases of change in behavior, clinicians need to consider possible medical causes such as hypothyroidism, urinary tract infections, constipation and pain. The Cornell Scale for Depression in Dementia can be used in these patients. A score greater than 12 indicates depression.
The Cornell Scale for Depression in Dementia
A = unable to evaluate
0 = absent
1 = mild or intermittent
2 = severe
| Mood-Related Signs | |
|---|---|
| 1. Anxiety (anxious expression, ruminations, worrying) | A 0 1 2 |
| 2. Sadness (sad expression, sad voice, tearfulness) | A 0 1 2 |
| 3. Lack of reactivity to pleasant events | A 0 1 2 |
| 4. Irritability (easily annoyed, short-tempered) | A 0 1 2 |
| Behavioral Disturbance | |
| 5. Agitation (restlessness, handwringing, hairpulling) | A 0 1 2 |
| 6. Retardation (slow movements, slow speech, slow reactions | A 0 1 2 |
| 7. Multiple physical complaints (score 0 if GI symptoms only) | A 0 1 2 |
| 8. Loss of interest (less involved in usual activities) (score only if change occurred acutely, ie. in less than 1 month) | A 0 1 2 |
| Physical Signs | |
| 9. Appetite loss (eating less than usual) | A 0 1 2 |
| 10. Weight loss (score 2 if greater than 5 pounds in 1 month) | A 0 1 2 |
| 11. Lack of energy (fatigues easily, unable to sustain activities) (score only if change occurred acutely, ie. in less than 1 month) | A 0 1 2 |
| Cyclic Functions | |
| 12. Diurnal variation of mood (symptoms worse in the morning) | A 0 1 2 |
| 13. Difficulty falling asleep (later than usual for this individual) | A 0 1 2 |
| 14. Multiple awakenings during sleep | A 0 1 2 |
| 15. Early-morning awakening (earlier than usual for this individual) | A 0 1 2 |
| Ideational Disturbance | |
| 16. Suicide (feels life is not worth living, has suicidal wishes, or makes suicide attempt) | A 0 1 2 |
| 17. Poor self-esteem (self-blame, self-deprecation, feelings of failure) | A 0 1 2 |
| 18. Pessimism (anticipation of the worst) | A 0 1 2 |
| 19. Mood-congruent delusions (delusions of poverty, illness, or loss) | A 0 1 2 |
Elder patients have a greater determination to die, give fewer warnings, use more violent and deadly methods to commit suicide, do more planning, have greater resolve and complete suicide at a higher rate. Suicide is the 13th leading cause of death in elders in the U.S. The incidence is 62/100,000 in white men — guns were used 71% of the time.
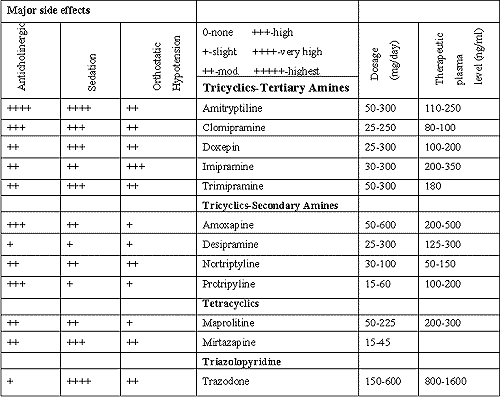
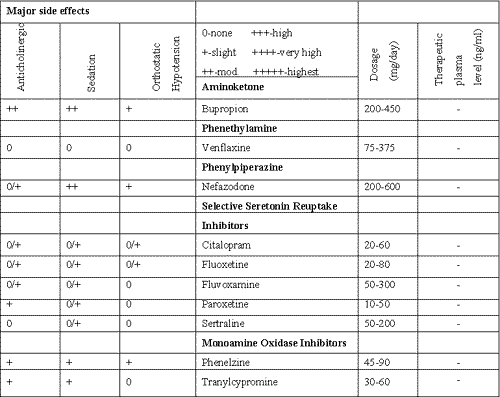
A literature review for 1995 to 2001 produced 33,167 subjects with a mean age of 72. Ninety-seven studies reported on antidepressants and 12 on electroconvulsive therapy. Eleven studies compared tricyclic antidepressants versus therapy with selective serotonin reuptake inhibitors (SSRIs). Eight of the studies showed equal efficacy and three showed that tricyclics were better. All types of antidepressants were tolerated well. Side effect profile was similar for all classes of antidepressants, although in some studies SSRIs had a better side effect profile (Table 1).
Treatment of the frail elderly must be monitored closed because they are more prone to side effects from antidepressants. In demented patients, some studies showed SSRIs and tricyclics, as compared to placebo, were equally effective but most showed no benefit. If patients are not responding to treatment, switching to a different class of antidepressant has been shown to be efficacious.
Electroconvulsive therapy (ECT), electric shock to the brain that produces a seizure, is the first choice in persons who are suicidal or who have severe weight loss, and ECT has been shown to be more effective than antidepressants. In a few studies, estrogen and methylphenidate demonstrated possible benefits. Psychotherapy in addition to medical therapy is better than medical therapy by itself. Finally, stimulation of the vagus nerve is being used experimentally to treat depression, as is electromagnetic brain stimulation.